Kyphoplasty
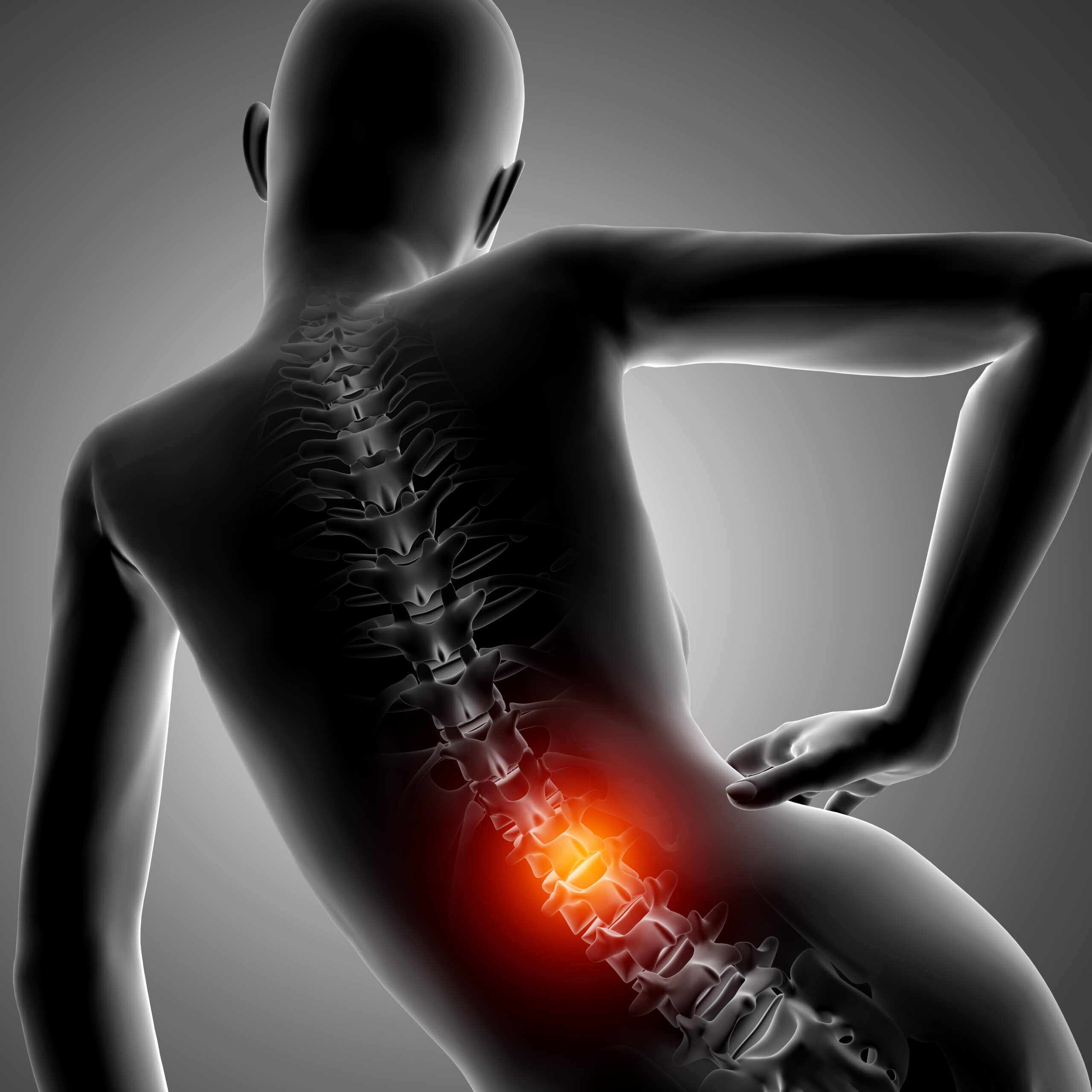
Kyphoplasty
Kyphoplasty is a minimally invasive procedure to treat compression fractures in the spine. These tiny fractures often happen in weakened vertebrae (commonly from osteoporosis or trauma) and can cause severe back pain and a hunched posture.
During kyphoplasty, the specialist inserts a balloon-like device into the collapsed vertebra and inflates it to create space, then fills that space with medical bone cement. The cement hardens quickly, stabilizing the fracture and often restoring some of the lost vertebral height.
This procedure is a type of vertebral augmentation, meaning it strengthens the broken bone from within.
Who is it for?
Kyphoplasty is typically recommended for patients with painful vertebral compression fractures, especially if the fracture is recent and causing significant pain or immobility. The most common candidates are older adults with osteoporosis-related fractures. It can also be used for fractures caused by certain spinal tumors. (metastatic cancer weakening the bone)
If you have sudden onset back pain after minor strain (like picking something up) or no specific injury and an X-ray or MRI shows a compression fracture, kyphoplasty might be an option. Ideal candidates have pain that correlates with the fracture, and imaging confirming the fracture’s presence.
If the fracture is old and already healed, kyphoplasty isn’t needed. Also, if you have multiple fractures or other spinal issues, our provider will evaluate if treating one level will significantly help your pain. We usually do kyphoplasty within the first 8 weeks of a fracture for best results, but sometimes later if pain persists.
What to Expect – Before, During, After
OneTreeHealth
You’ll have an evaluation including imaging (usually an MRI or X-ray) to locate the fracture. We’ll ensure the fracture is the source of pain (sometimes we do a diagnostic injection). Once confirmed, we schedule the kyphoplasty. Because it’s minimally invasive, it’s often done in an outpatient setting or a short hospital stay. You may get basic blood tests beforehand. We’ll instruct you to stop certain medications (like blood thinners) a few days prior. The night before, no eating or drinking after midnight if the procedure will use sedation or anesthesia. Arrange a ride, as you won’t be driving after.
OneTreeHealth
Kyphoplasty usually takes about an hour (give or take 30 minutes depending on number of fractures treated). You’ll lie face-down on a special table. You might receive either local anesthesia with mild sedation or light general anesthesia – our anesthesia team will discuss the best option. After numbing the skin and tissue, the doctor inserts a hollow needle (trocar) through a tiny incision in your back into the fractured vertebra, guided by X-ray (fluoroscopy).
Through the needle, a small balloon is inserted and inflated, which pushes the broken bone pieces back toward normal alignment and creates a cavity. The balloon is then deflated and removed, and medical-grade bone cement is slowly injected into the cavity. You won’t feel the cement, and we closely monitor to ensure it stays in the bone. The cement hardens in minutes, stabilizing the fracture. Then the needle is removed. Usually only a bandage is needed – no stitches.

OneTreeHealth
You’ll spend maybe an hour or two in recovery lying flat while the anesthesia wears off. We’ll monitor your vital signs and make sure you feel okay. Often patients can feel a reduction in their back pain as soon as they stand up, or within the first day – it can be quite dramatic. You’ll likely be able to go home the same day. We advise taking it easy for the rest of that day; you can usually resume light activities the next day. You might have soreness at the needle site, which is usually mild.
We’ll schedule a follow-up appointment and possibly a follow-up X-ray to see the cement placement. And we’ll talk about preventing future fractures (like treating osteoporosis with calcium, Vitamin D, medications, etc.). We also caution avoiding heavy lifting or jarring activities for a few weeks to allow the area to settle.
Benefits
The primary benefit is rapid pain relief and stabilization. Kyphoplasty often significantly reduces back pain caused by the fracture, letting you get back on your feet sooner.
By restoring vertebral height, it can also improve spine alignment and prevent that “hunched” deformity (kyphosis) that can happen with multiple fractures. Early mobility helps avoid complications of being bedridden (like blood clots or pneumonia).
It’s minimally invasive – only tiny incisions, no large open surgery, so recovery is quick and infection risk is low. Many patients avoid or reduce their need for pain medications after kyphoplasty because their pain improves.
Risks
Kyphoplasty is generally safe, but there are some risks. There’s a small risk of infection (as with any procedure involving needles – roughly under 1%). Bleeding risk is minimal, but we still take precautions, especially if you were on blood thinners. A unique risk is cement leakage – sometimes a bit of cement can leak out of the bone into surrounding areas.
We carefully monitor under X-ray to minimize this. In rare cases, leaked cement could press on nerves or blood vessels, potentially requiring surgery to remove it, but this is uncommon. There’s also a very small risk of an allergic reaction to any of the materials or medications used.
Adjacent vertebra fracture is another consideration:
some studies have noted that if you have one fracture, others can occur later (due to underlying osteoporosis), though whether kyphoplasty increases that risk is debated. We mitigate risks by proper patient selection, using experienced technique, and monitoring closely during the procedure.
Frequently Asked Questions:
Kyphoplasty often provides significant relief if your pain is truly from the compression fracture. Many patients report their pain goes from a severe level
down to mild or none. However, if you have other spine issues (arthritis, disc
problems), you might still have some baseline back ache. It specifically
addresses fracture pain. We will evaluate you to be sure the fracture is the main
pain source. If it is, you can expect notable improvement. Some soreness from
the procedure can exist for a couple days, but that’s usually minor compared to
the original pain.
One of the great things about kyphoplasty is the quick recovery. You’ll likely be up and walking the same day. We usually advise avoiding very strenuous activity or heavy lifting for about 2 weeks to be cautious. But you can do light daily activities as tolerated – getting around the house, gentle walks, etc., even the next day. If your job is sedentary, you might return in a few days; if it’s physical, perhaps a couple weeks off. Everyone’s pain relief timeline is a bit different, but many feel a big improvement right away. We will give individualized guidance. Also, we’ll likely get you started on osteoporosis treatment if applicable to protect the rest of your bones moving forward.
We can treat more than one level if needed. Often we can address two vertebrae in one session if they’re adjacent. If you have several, we might stage them (do two now, maybe another later) depending on your situation. Each case is unique. Our goal is to give you the most relief with the least risk. We’ll formulate a plan if multiple areas are involved.



Contact Us Today!
Don’t endure weeks of bedrest and pain if you don’t have to.
If you’re suffering from a painful spinal compression fracture, kyphoplasty could be a game-changer.
Contact One Tree Health’s Interventional Pain specialists to find out if you’re a candidate for kyphoplasty. We’ll provide a thorough evaluation and discuss the best approach to get
you standing tall again. Schedule an appointment today and take the first step towards relief from fracture pain.
OneTreeHealth provides coordinated, compassionate care for patients recovering from injury specializing in orthopaedics, neurology, surgery, interventional pain management, and more. We simplify the recovery journey by managing care under one roof, so patients can focus on healing.
Useful Links
Reach Us
397 Wallace Rd Nashville, TN 37211 Suite#303
(615) 696-9900
hello@onetreehealth.com
Copyright 2025, One Tree Healthcare. All Rights Reserved.

