Epidural Steroid
Injection
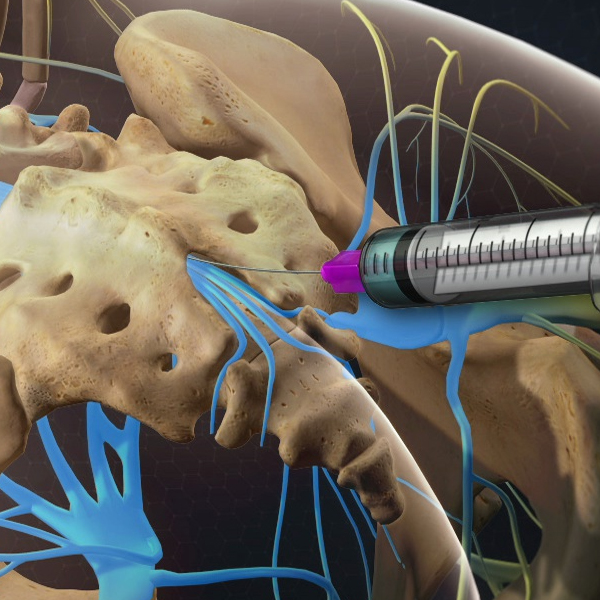
What is an Epidural Steroid Injection?
An Epidural Steroid Injection (ESI) is a common pain management procedure where a mixture of a corticosteroid (anti-inflammatory medicine) and anesthetic is injected into the epidural space around the spinal nerves. The goal is to reduce inflammation and swelling around irritated nerves in your spine, which in turn can alleviate pain radiating to your arms or legs. Think of it as delivering potent relief right to the source of nerve pain. ESIs can be done in the cervical (neck), thoracic (upper back), or lumbar (lower back) spine depending on where your symptoms are. By calming down inflamed nerves – such as those pinched by a herniated disc or narrowed foramina – an ESI can provide pain relief that lasts for weeks to months.
Who is it for?
ESIs are often recommended for radicular pain – that is, pain that travels down an arm or leg along the path of a nerve (commonly called sciatica when in the leg). If you have a herniated disc pressing on a nerve root, spinal stenosis causing leg pain, or even a flare-up of chronic back pain with nerve irritation, an ESI might help.
For example, candidates include:
![]() A person with a lumbar disc herniation causing sciatica (shooting leg pain, numbness, maybe foot drop).
A person with a lumbar disc herniation causing sciatica (shooting leg pain, numbness, maybe foot drop).
![]() Someone with spinal stenosis who gets leg pain when walking (neurogenic claudication).
Someone with spinal stenosis who gets leg pain when walking (neurogenic claudication).
![]() A patient with cervical disc bulge causing arm pain and tingling.
A patient with cervical disc bulge causing arm pain and tingling.
![]() Sometimes, even for thoracic pain like a shingles outbreak (herpes zoster) or certain chronic pain syndromes, an epidural can provide relief.
Sometimes, even for thoracic pain like a shingles outbreak (herpes zoster) or certain chronic pain syndromes, an epidural can provide relief.
We usually consider an ESI when conservative measures (rest, medications, therapy) haven’t fully helped and before considering surgery. It’s also used as a part of a rehab plan – relieving pain enough so you can participate in physical therapy. It can also be diagnostic: if you get relief, it confirms the nerve level causing the problem. However, ESIs are not typically for general low back pain without a nerve component (they work best for nerve-related pain).
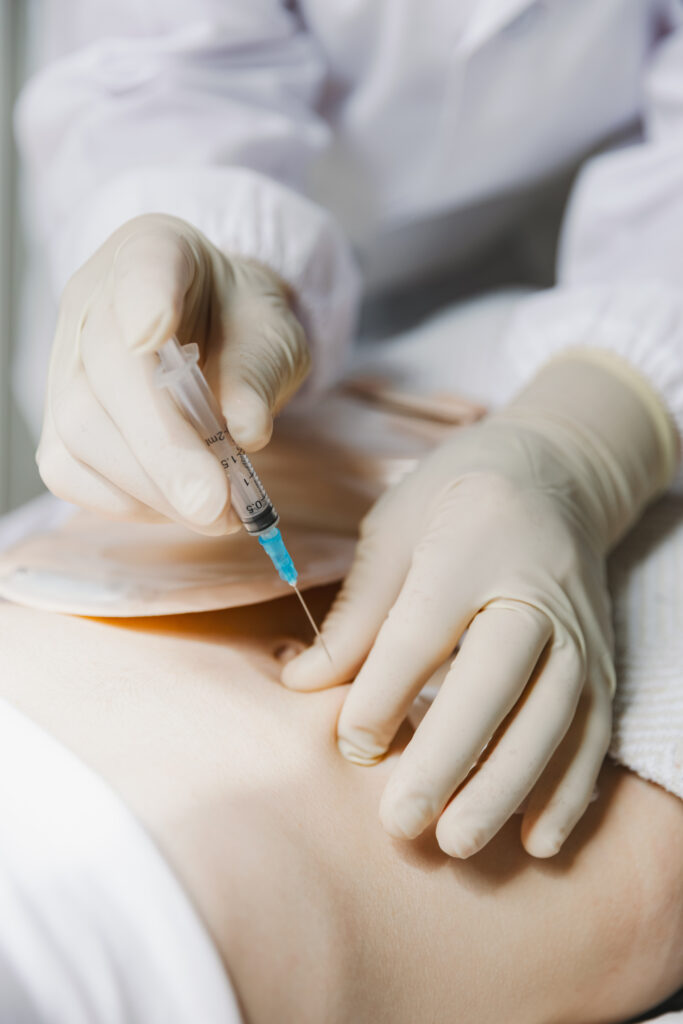
What to Expect – Before, During, After
OneTreeHealth
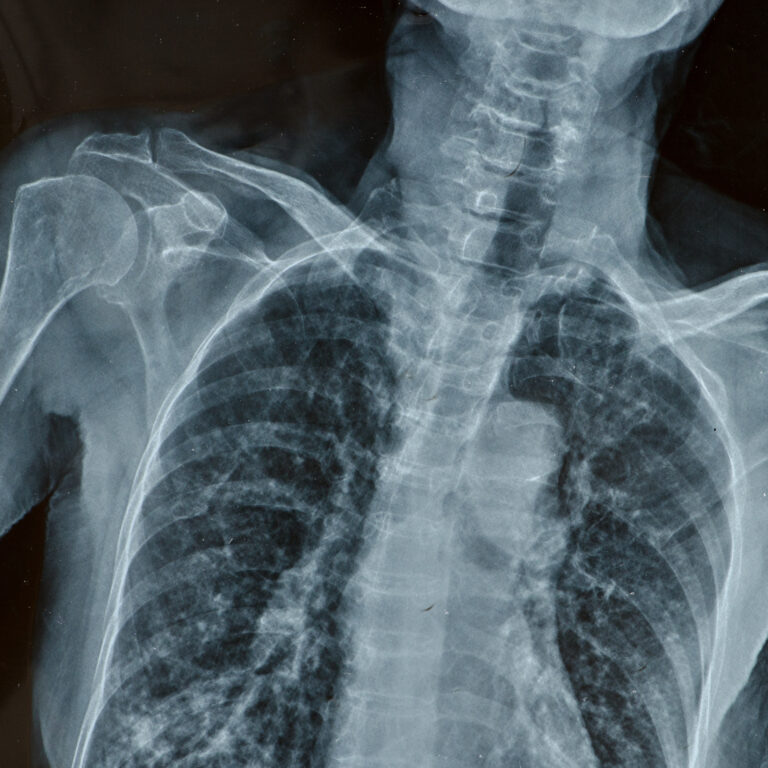
We’ll review your MRI/CT scans to target the injection level. We ensure you don’t have contraindications (like infection or uncontrolled diabetes – as steroids can raise blood sugar). If you’re on blood thinners, we’ll coordinate holding them for a few days prior (safety to avoid bleeding). On the day, you caneat a light meal unless told otherwise.
You’ll change into a gown. We discussrisks and you’ll sign consent. Typically, you lie on an X-ray table for the procedure (face down for lumbar, maybe face down or seated for cervical). Sedation is usually minimal – most ESIs are done with local anesthetic only, but if you’re very anxious we might give a small dose of relaxing medication (not full anesthesia).
OneTreeHealth
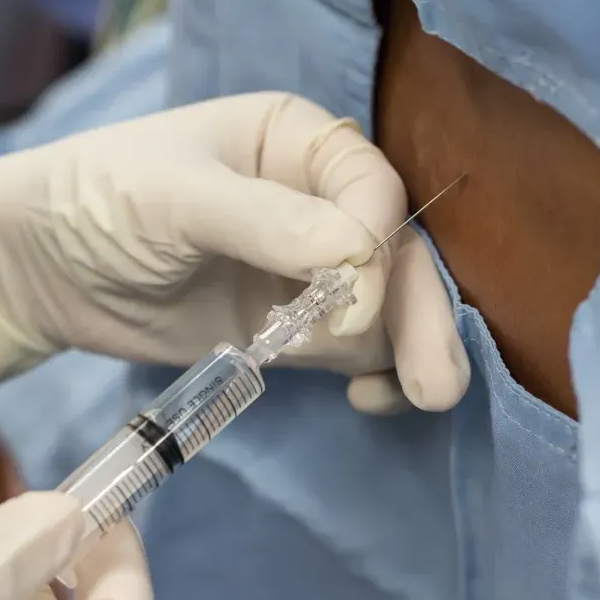
The skin over the injection site is cleaned thoroughly and numbed with a local anesthetic needle (a quick pinch and burn). Using fluoroscopy (live X-ray), the doctor guides a spinal needle into the epidural space – which is just outside
the covering of the spinal cord, where nerves run and where inflammation happens.
You might feel some pressure but sharp pain is minimized by the numbing. We often do a test with a tiny bit of contrast dye to ensure proper placement (you might feel a pressure in your back or down your leg briefly). Then the steroid/anesthetic solution is slowly injected. Sometimes you’ll feel a fullness or pressure in the back, or even a replica of your sciatic pain (as the medicine flows around the nerve) – inform us of what you feel; it’s useful feedback and usually not severe.
The injection itself is quick, maybe a few minutes. Then the needle is removed and a bandage applied. The whole procedure takes about 10- 15 minutes, plus setup time.

OneTreeHealth
You’ll be monitored for 15-30 minutes before going home. We check your blood pressure, etc., especially if any sedation was given. It’s normal to feel some immediate numbness or even a reduction in pain in the affected area due to the local anesthetic – that might wear off in a few hours. Conversely, some people feel a temporary “pressure” or even a slight increase in pain for a day as the steroid starts to work. We advise taking it easy the rest of the day – no strenuous activity.
You can resume normal light activities the next day. The steroid generally takes 2-3 days to start reducing inflammation, and peak relief might be about a week after injection. We’ll have you keep a pain diary and follow up in a couple of weeks to gauge results. You may be a bit sore at the injection site – ice can help that. We typically recommend not submerging in water (pool, bath) for 24-48 hours to reduce infection risk, but showering is fine next day.
Depending on the outcome, some patients may need a series of injections (often up to 3, spaced a few weeks apart) for maximal benefit, but others get enough relief from just one.
Benefits
The main benefit is significant pain relief without surgery, allowing you to improve function and participate in rehab. By reducing nerve inflammation, ESIs can ease radiating arm/leg pain, numbness, or tingling. Many patients experience improvement in their ability to walk, sleep, or sit comfortably.
The relief can last for several weeks or even months; sometimes one injection “calms things down” enough that the body heals the issue (like the disc shrinks) and pain doesn’t return. It’s also outpatient, low risk, and quick to perform. If it works, it might help you avoid or delay the need for an operation. Additionally, it can confirm that we’re treating the correct level – a diagnostic bonus.
Risks
ESIs are generally very safe when done by experienced hands, but here are potential risks:
<img src="https://www.onetreehealth.com/wp-content/uploads/2025/08/CITYPNG.COMHD-Circle-Green-Tick-Mark-Symbol-Icon-PNG-1500x1500-1-300x300.png" alt="" width="31" height="31" Common but minor: Temporary soreness at injection site, transient headache (especially if a dural puncture occurs leading to CSF leak; we take precautions to avoid this by proper technique).
<img src="https://www.onetreehealth.com/wp-content/uploads/2025/08/CITYPNG.COMHD-Circle-Green-Tick-Mark-Symbol-Icon-PNG-1500x1500-1-300x300.png" alt="" width="31" height="31" Infection: Very rare (<0.1%), since it’s a sterile procedure. To mitigate, we use full sterile prep and equipment.
<img src="https://www.onetreehealth.com/wp-content/uploads/2025/08/CITYPNG.COMHD-Circle-Green-Tick-Mark-Symbol-Icon-PNG-1500x1500-1-300x300.png" alt="" width="31" height="31" Bleeding: Also rare, but if on blood thinners or have a bleeding disorder, bleeding in the epidural space could theoretically cause pressure on nerves (epidural hematoma). That’s why we ensure normal coagulation before injecting.
<img src="https://www.onetreehealth.com/wp-content/uploads/2025/08/CITYPNG.COMHD-Circle-Green-Tick-Mark-Symbol-Icon-PNG-1500x1500-1-300x300.png" alt="" width="31" height="31" Nerve Injury: Direct damage to nerves is extremely rare, as we don’t usually touch the nerve (we’re in the space around them). But if a nerve root is very irritated, sometimes the injection can temporarily “tickle” it causing a zing sensation.
<img src="https://www.onetreehealth.com/wp-content/uploads/2025/08/CITYPNG.COMHD-Circle-Green-Tick-Mark-Symbol-Icon-PNG-1500x1500-1-300x300.png" alt="" width="31" height="31" Steroid-related: Steroids can cause side effects – a temporary rise in blood sugar (diabetics need to monitor), facial flushing, insomnia for a night or two, or in rare cases, effects like mood changes. These are usually short-lived because it’s a one-time dose (or limited series).
<img src="https://www.onetreehealth.com/wp-content/uploads/2025/08/CITYPNG.COMHD-Circle-Green-Tick-Mark-Symbol-Icon-PNG-1500x1500-1-300x300.png" alt="" width="31" height="31" Dural Puncture (“spinal headache”): If the needle accidentally goes a bit too deep and punctures the sac (dura) holding spinal fluid, you might get a headache after (worse when sitting/standing). It’s not common; if it happens and doesn’t resolve with fluids and rest, we can treat it (with a blood patch). We strive to avoid this by careful technique and using the appropriate needles.
<img src="https://www.onetreehealth.com/wp-content/uploads/2025/08/CITYPNG.COMHD-Circle-Green-Tick-Mark-Symbol-Icon-PNG-1500x1500-1-300x300.png" alt="" width="31" height="31" No relief: Unfortunately, not everyone responds to an ESI. If it doesn’t help, we reevaluate your condition – either the issue may not be inflammation-based or the level might have been off target. Sometimes a repeat injection yields more info or relief.
Overall, serious complications are very uncommon, and we believe the potential benefit outweighs these risks in indicated patients. We’ll discuss all these with you beforehand so you’re informed.
Frequently Asked Questions:
It varies. Some patients get relief that lasts months or even permanently for that episode (especially if combined with fixing the root cause and therapy). Others might feel great for a while but then symptoms slowly return after a few weeks. Generally, the goal is to get several weeks of relief at least, during which time you can heal and strengthen. If pain returns, we can consider another injection.
We usually don’t do more than 3 injections in a 6-12 month period focused on one area, due to diminishing returns and steroid dose limits. Every individual responds differently. We’ve seen patients break a pain cycle with one shot and never need another, and others who come periodically for maintenance injections.
Not directly – it doesn’t make a big disc herniation disappear (surgery or time does that), but it reduces the inflammation and pain so that your body can often mend on its own. Discs can shrink over time. If you can stay active and do therapy because you’re not in severe pain, that helps recovery. So, think of it as symptom control and a window of opportunity for natural healing. In some cases, if the underlying structural issue is severe (huge disc fragment, severe stenosis), an injection may only be a temporary bridge and surgery might still be needed. But many times it’s enough to avoid surgery.
We do our best to minimize discomfort. The initial numbing injection stings for a few seconds. After that, you feel pressure rather than sharp pain. If you feel anything sharp or a jolt during, let us know – we adjust the needle or give more numbing. Most patients tolerate it well and say it’s not as bad as they expected, often rating it mild to moderate discomfort, not severe. If you’re especially anxious, mild sedation can be arranged, but then you’d need someone to drive you and a bit longer recovery. Typically, it’s over so fast that patients do fine with just local anesthetic.
If one injection gives partial relief, we might do a second one in 2 weeks to compound the effect. If it gives no relief at all, we’d reexamine the diagnosis: maybe the pain isn’t from nerve inflammation (for example, could it be hip arthritis referring to the leg, etc.). Or maybe the level injected wasn’t the right one (rare if imaging correlates well, but sometimes multiple levels). We may try another at a neighboring level if clinically indicated.
If after a couple attempts there’s no improvement, then ESIs are likely not the solution for your case, and we’d pivot to other treatments (different injection types, medications, or surgical consult depending on the issue). Our aim is to use the right tool for the job – we’ll reassess if needed.
No heavy exercise or strenuous activity on the same day – just rest. From the next day, you can gradually resume activities. We often tell patients to listen to their body – if you feel good, you can do more, but don’t overdo it immediately. Keep walking, do gentle movements, but avoid heavy lifting or twisting for a couple days as the medication settles in.
If you are in physical therapy, we might have you skip a day or two after injection then continue. Most people can fully return to their normal routine by 24-48 hours post injection. You might feel so good you want to catch up on chores – still take it easy at first to avoid flaring things up. And, keep taking any prescribed medications unless directed otherwise.



Contact Us Today!
Don’t let sciatica or nerve pain control your life - take control of it.
If nerve pain is running down your arm or leg and holding you back, an Epidural Steroid Injection might offer you the relief you need to get moving again. At One Tree Health, our experts perform ESIs safely and effectively, targeting the source of your pain. Contact us today to schedule a consultation for an epidural injection. We’ll answer your questions, evaluate your condition, and, if appropriate, provide this treatment to help you feel better fast.
Schedule an Appointment with our pain management specialists and start your journey to relief now.
OneTreeHealth provides coordinated, compassionate care for patients recovering from injury specializing in orthopaedics, neurology, surgery, interventional pain management, and more. We simplify the recovery journey by managing care under one roof, so patients can focus on healing.
Useful Links
Reach Us
397 Wallace Rd Nashville, TN 37211 Suite#303
(615) 696-9900
hello@onetreehealth.com
Copyright 2025, One Tree Healthcare. All Rights Reserved.

