Nerve Block
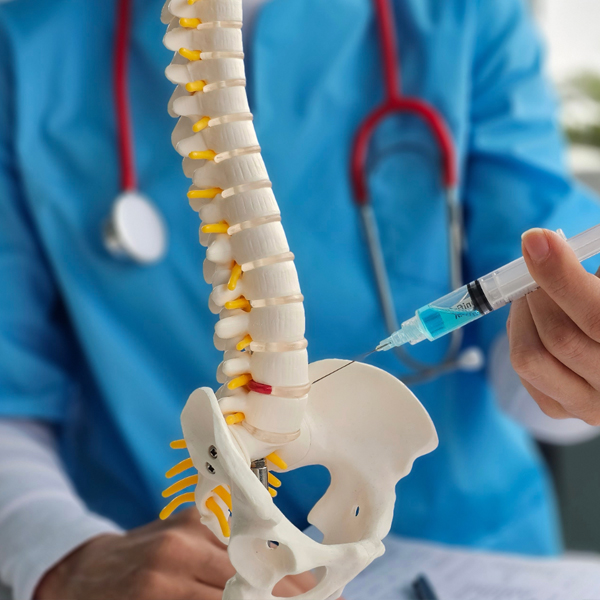
What is a Nerve Block?
A Nerve Block is a procedure in which an anesthetic (numbing medicine) – often combined with an anti-inflammatory like a steroid – is injected around or near a specific nerve or group of nerves to block pain signals from traveling to the brain . Think of it as putting a roadblock on the pain pathway. Nerve blocks can be done on many different nerves throughout the body, depending on where your pain is. They can provide temporary relief (hours to months, depending on the medications used) and are used both diagnostically (to confirm a suspected pain source) and therapeutically (to relieve pain).
Some common examples: a facet joint medial branch block (for spine pain), an occipital nerve block (for headaches), a stellate ganglion block (for complex regional pain or arm pain), or peripheral nerve blocks like a suprascapular nerve block (for shoulder pain), among many othersnuvancehealth.org.
Who is it for?
Nerve blocks are versatile, used for acute and chronic pain conditions. You might be a candidate if you have pain that can be traced to a specific nerve or nerve cluster.
Situations include:
![]() Diagnostic blocks: You have undiagnosed pain and doctors suspect a particular nerve is causing it. A block can confirm by temporarily numbing that nerve to see if pain goes away.
Diagnostic blocks: You have undiagnosed pain and doctors suspect a particular nerve is causing it. A block can confirm by temporarily numbing that nerve to see if pain goes away.
![]() Therapeutic blocks: Chronic pain like Complex Regional Pain Syndrome (CRPS) in a limb – a sympathetic nerve block can ease pain and improve circulationg. Or post-surgical nerve pain – a peripheral nerve block might calm it.
Therapeutic blocks: Chronic pain like Complex Regional Pain Syndrome (CRPS) in a limb – a sympathetic nerve block can ease pain and improve circulationg. Or post-surgical nerve pain – a peripheral nerve block might calm it.
![]() Facet or Epidural Blocks: As discussed earlier, these are essentially nerve blocks of spinal nerves (medial branch blocks, transforaminal blocks for sciatica, etc.).
Facet or Epidural Blocks: As discussed earlier, these are essentially nerve blocks of spinal nerves (medial branch blocks, transforaminal blocks for sciatica, etc.).
![]() Headaches/Migraines: e.g., Occipital nerve blocks for occipital neuralgia or migraine prevention.
Headaches/Migraines: e.g., Occipital nerve blocks for occipital neuralgia or migraine prevention.
![]() Visceral pain: e.g., a celiac plexus block for pancreatic cancer pain.
Visceral pain: e.g., a celiac plexus block for pancreatic cancer pain.
![]() Pre-surgery or Intraoperative: Often anesthesiologists do nerve blocks to provide anesthesia and post-op pain control for surgeries (like a brachial plexus block for arm surgery). That’s in the OR setting.
Pre-surgery or Intraoperative: Often anesthesiologists do nerve blocks to provide anesthesia and post-op pain control for surgeries (like a brachial plexus block for arm surgery). That’s in the OR setting.
At One Tree Health, we focus on blocks for pain management. If you have pain in a specific distribution (say the front of the thigh indicating femoral nerve, or the foot indicating tibial nerve), and imaging/clinical exam suggests that nerve, a block might help.
Also for patients not ready for RFA or surgery, a nerve block can buy time with relief.
What to Expect – Before, During, After

OneTreeHealth
Similar to other procedures, we’ll explain the plan and get consent. We review any meds (hold blood thinners if needed for certain deeper blocks). Depending on the block location, you might be sitting, lying on your stomach/back, or side. Ultrasound or fluoroscopy (X-ray) guidance is often used to precisely target the nerve.
No heavy sedation is usually needed, but we keep you comfortable. Area will be cleaned and prepped sterilely. You can usually eat lightly and take routine meds (except blood thinners) because sedation is minimal.
OneTreeHealth
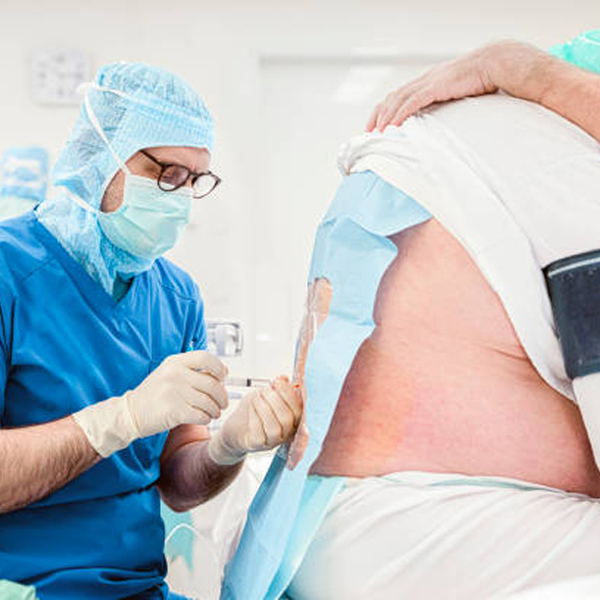
We apply a local anesthetic to the skin first. Then, using guidance (ultrasound is great for visualizing many peripheral nerves in real-time; X-ray is great for spine-related nerves), we advance a fine needle toward the nerve or nerve bundle. We might ask if you feel tingling in the area of your pain, which could indicate we’re near the nerve (some blocks use a nerve stimulator as well to confirm location by causing a muscle twitch).
Once in position, we slowly inject the medication. You might feel pressure or slight discomfort; if you do, let us know and we can adjust or go slower. For example, during a stellate ganglion block (neck region), you might feel some pressure in the neck or warmth in the face; for a lumbar sympathetic block, maybe warmth in the leg. The injection only takes a minute or two. After injecting, we withdraw the needle and put a band- aid. The immediate effect often is noticeable – e.g., the area might feel numb or the pain diminishes within minutes if a local anesthetic was used.

OneTreeHealth
We’ll monitor you for a short time. Depending on the block, we might check certain functions: e.g., after a stellate ganglion block, it’s expected to have drooping eyelid and red eye temporarily (Horner’s syndrome) indicating a successful block. After a lumbar plexus block, your leg may feel weak/numb for a few hours, so we’d caution against walking until it wears off.
Generally, plan to take it easy rest of the day, especially if something is numb – you don’t want to injure yourself inadvertently. Pain relief can last as long as the anesthetic lasts (a few hours) plus, if steroid was included, days to weeks as it reduces inflammation. Sometimes multiple blocks are needed to break the pain cycle. For diagnostic blocks, you’ll record your pain relief for the first few hours before it wears off (that’s the diagnostic info). We’ll give instructions specific to the block (like for a celiac plexus block: watch for any drops in blood pressure rest of day, which can happen due to autonomic changes). You’ll likely be able to return to most normal activities by the next day. We schedule any follow-up or additional blocks if part of a series.
Benefits
Nerve blocks can provide immediate pain relief, even if temporary, which is a blessing for someone in severe pain. This can allow you to function, go to therapy, or simply rest. Repeated therapeutic blocks sometimes have a cumulative effect (like a series of sympathetic blocks can dampen CRPS pain long-term).
For some acute issues, one block might even cure the problem if it allows the nerve to “reset” or heal. Diagnostically, blocks are invaluable for pinpointing pain generators, which then guides further treatment (like confirming it’s facet joint pain before doing RFA). They’re also less systemic than oral meds – targeted relief with less overall medication side effects. The procedures are quick and done with just a needle – no large incisions or hospital stays. Many times, nerve blocks can postpone or eliminate the need for more invasive treatments. And if a block works wonders, it opens the door to procedures like RFA for longer relief.
Risks
Risks vary with the site of the block, but general ones:
<img src="https://www.onetreehealth.com/wp-content/uploads/2025/08/CITYPNG.COMHD-Circle-Green-Tick-Mark-Symbol-Icon-PNG-1500x1500-1-300x300.png" alt="" width="31" height="31" Bleeding or Hematoma: Rare, but if a needle passes through a blood vessel (we try to avoid that with imaging), bleeding can occur. In highly vascular areas or those near critical structures (like a stellate ganglion block near neck vessels), precision is key. If you have a bleeding tendency, we might avoid certain blocks.
<img src="https://www.onetreehealth.com/wp-content/uploads/2025/08/CITYPNG.COMHD-Circle-Green-Tick-Mark-Symbol-Icon-PNG-1500x1500-1-300x300.png" alt="" width="31" height="31" Infection: Very low risk due to sterile technique, but any injection through skin carries a small chance. We make sure no active infection is present and use sterile prep.
<img src="https://www.onetreehealth.com/wp-content/uploads/2025/08/CITYPNG.COMHD-Circle-Green-Tick-Mark-Symbol-Icon-PNG-1500x1500-1-300x300.png" alt="" width="31" height="31" Nerve Injury: We are targeting near nerves, so there’s a slight risk of direct trauma or irritation to the nerve. This could cause increased pain, numbness, or (very rarely) weakness. Using imaging and proper technique mitigates this. Usually, any irritation is temporary.
<img src="https://www.onetreehealth.com/wp-content/uploads/2025/08/CITYPNG.COMHD-Circle-Green-Tick-Mark-Symbol-Icon-PNG-1500x1500-1-300x300.png" alt="" width="31" height="31" Temporary Numbness/Weakness: As expected, because we numbed the nerve. For instance, a femoral nerve block will make your quadriceps weak for a few hours; you must be careful or use crutches until it wears off. This is expected and wears off as the anesthetic does.
<img src="https://www.onetreehealth.com/wp-content/uploads/2025/08/CITYPNG.COMHD-Circle-Green-Tick-Mark-Symbol-Icon-PNG-1500x1500-1-300x300.png" alt="" width="31" height="31" Allergic reaction: Rare if any, mostly if someone is allergic to the local anesthetic (like lidocaine) – we screen for that.
<img src="https://www.onetreehealth.com/wp-content/uploads/2025/08/CITYPNG.COMHD-Circle-Green-Tick-Mark-Symbol-Icon-PNG-1500x1500-1-300x300.png" alt="" width="31" height="31" Systemic effects: If a large amount of anesthetic inadvertently entered the bloodstream, it could cause systemic toxicity (like affecting the heart or brain). But we use safe doses, aspirate to check we’re not in a vessel, and use incremental injection techniques to avoid this. Also, specific blocks have unique side effects: e.g., stellate ganglion can cause temporary hoarse voice or a feeling of a lump in throat (due to nerve involvement) – these wear off.
<img src="https://www.onetreehealth.com/wp-content/uploads/2025/08/CITYPNG.COMHD-Circle-Green-Tick-Mark-Symbol-Icon-PNG-1500x1500-1-300x300.png" alt="" width="31" height="31" Not effective: The block might not relieve pain if we didn’t hit the exact right spot or if that nerve wasn’t actually the pain source. This trial and error is sometimes part of diagnostic blocks. We refine our approach based on results.
Overall, nerve blocks are low-risk when done carefully, but we always tailor the approach to the patient’s anatomy and needs. We discuss any specific risk that might apply to the nerve we’re blocking ahead of time.
Frequently Asked Questions:
The numbing effect from the local anesthetic will last a few hours typically (depending on which drug used, maybe 4-8 hours). If we include steroid, the pain relief from reduced inflammation might start later that day or the next day and could last a few days to several weeks. Some purely diagnostic blocks use only anesthetic (so relief is just hours) – that’s to see if pain returns when it wears off, confirming the source.
Therapeutic blocks often combine steroid for longer relief. Some nerve blocks (like in CRPS) repeated in series can extend relief more each time. But generally, for a single block, don’t expect more than a couple weeks from one injection, if steroid is used, and just hours if not. Each situation is different though.
We do our best to make it as comfortable as possible. You’ll feel a quick pinch from the numbing needle. Pressure sensations during the block are common. If we’re near a nerve, sometimes there’s a momentary zing or reproduction of your pain – that can actually be a sign we’re in the right spot, ironically. We warn patients of that possibility (“you might feel your usual pain shoot briefly – it means we’re touching the nerve causing it”). We will minimize any sharp pains.
The procedure is usually over in just a few minutes, and most patients tolerate it quite well. Many blocks are no more uncomfortable than a typical shot or blood draw after the numbing is done.
Follow any specific instructions we give you. Generally, take it easy the day of. If your leg was numbed, you must be careful not to fall – don’t bear weight until sensation returns. You might use a sling if an arm is numbed to avoid letting it dangle. Keep the injection site clean and dry for a day. Watch for any concerning signs like swelling, redness (rare signs of infection) or if you had a sympathetic block watch for any unusual symptoms. But mostly, rest and enjoy the relief!
We also advise you to not do something extreme just because you’re numb (like if your shoulder block took away pain, don’t go lift heavy stuff that evening because you could injure yourself without feeling it). Once sensation/pain returns, use that information: if it was diagnostic, note how much and how long relief you got. If therapeutic, continue any other treatments (e.g., physical therapy) as directed, hopefully now with less pain.
Yes, depending on the situation. For some conditions, a series of blocks is planned. We always weigh the benefits of repeat injections, especially with steroids (too many steroids can have systemic effects). But spaced out appropriately, multiple blocks can be fine. Some patients with chronic issues get them periodically for flare-ups. We might try a block in one area, then another if diagnosing. If a block gives only partial relief, a repeat might boost it.
However, if you need very frequent blocks to manage pain, we might consider more definitive options like RFA or surgery. Each block usually must be at least a week or two apart if repeating, to allow assessment and avoid overlap of steroid dosing.
If a properly placed nerve block gives no relief, it suggests either that nerve isn’t the source of pain or something else is overriding the pain. We’d go back to the diagnostic drawing board. Sometimes it means the pain might be more central or from multiple sources.
We might try a different block or different approach. It’s valuable information – a negative block can rule out a diagnosis. Of course, if it doesn’t help, we won’t keep doing the same block. We’ll discuss other tests or referrals. It’s all about narrowing down what will improve your pain.



Contact Us Today!
A precise nerve block could be the key to unlocking your pain relief.
Whether it’s severe headaches, back pain, or complex regional pain, our specialists at One Tree Health can pinpoint and block the nerves causing your discomfort. Experience the relief of a targeted treatment that can help you return to normal activities without the constant pain.
Contact One Tree Health to learn if a nerve block is right for you. We will carefully evaluate your pain pattern and recommend the appropriate block if it’s indicated. Don’t let pain dictate your day – take control with the help of our advanced pain management techniques.
Schedule a consultation now and step onto the path of relief.
OneTreeHealth provides coordinated, compassionate care for patients recovering from injury specializing in orthopaedics, neurology, surgery, interventional pain management, and more. We simplify the recovery journey by managing care under one roof, so patients can focus on healing.
Useful Links
Reach Us
397 Wallace Rd Nashville, TN 37211 Suite#303
(615) 696-9900
hello@onetreehealth.com
Copyright 2025, One Tree Healthcare. All Rights Reserved.

