Discectomy
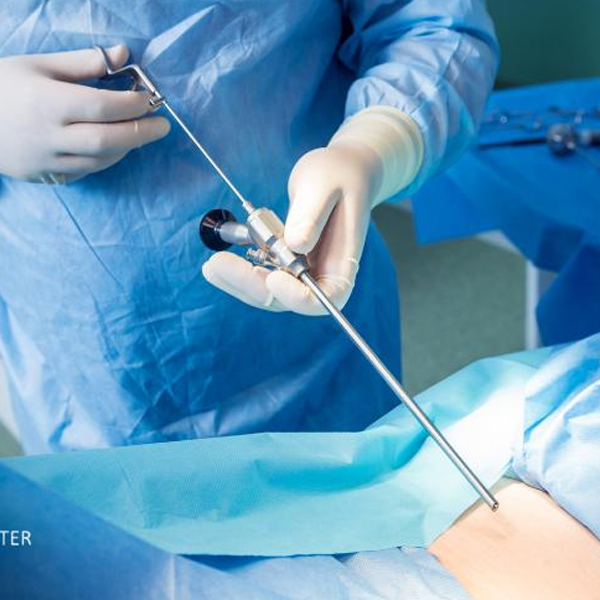
Discectomy
A Discectomy is a surgical procedure to remove part of a damaged intervertebral disc that is pressing on a nerve or the spinal cord. Typically, it refers to removing a herniated portion of a disc (the soft cushion between vertebrae) that has bulged or extruded out and is causing nerve compression. By taking out the offending disc fragment, the pressure on the nerve is relieved, which can alleviate pain, numbness, or weakness in the area that nerve controls.
The most common form is a Lumbar Microdiscectomy for sciatica (leg pain from a herniateddisc in the lower back). It can also be done in the neck (cervical discectomy, often aspart of an ACDF – anterior cervical discectomy and fusion). The term “microdiscectomy”is often used because these days surgeons use minimally invasive techniques and a microscope or loupes to perform it through a small incision.
Who is it for?
Patients who typically benefit from discectomy are those with:
![]() A confirmed herniated disc on MRI/CT that correlates with symptoms (e.g., herniation at L5-S1 compressing S1 nerve root causing sciatica down the back of the leg).
A confirmed herniated disc on MRI/CT that correlates with symptoms (e.g., herniation at L5-S1 compressing S1 nerve root causing sciatica down the back of the leg).
![]() Significant leg or arm pain (radiculopathy) that has not improved with conservative treatments like medications, physical therapy, or steroid injections, usually over a period of at least several weeks.
Significant leg or arm pain (radiculopathy) that has not improved with conservative treatments like medications, physical therapy, or steroid injections, usually over a period of at least several weeks.
![]() Or those with severe symptoms or neurological deficits: such as significant weakness (foot drop, etc.) or very severe pain where waiting is intolerable.
Or those with severe symptoms or neurological deficits: such as significant weakness (foot drop, etc.) or very severe pain where waiting is intolerable.
![]() In emergency cases like cauda equina syndrome (when a large disc herniation causes bowel/bladder dysfunction and saddle anesthesia), an urgent discectomy is done to prevent permanent damage.
In emergency cases like cauda equina syndrome (when a large disc herniation causes bowel/bladder dysfunction and saddle anesthesia), an urgent discectomy is done to prevent permanent damage.
![]() Generally, if leg pain is the dominant symptom and imaging shows a disc pushing on the corresponding nerve, and especially if it hurts more than back pain, discectomy has a high success rate for relief.
Generally, if leg pain is the dominant symptom and imaging shows a disc pushing on the corresponding nerve, and especially if it hurts more than back pain, discectomy has a high success rate for relief.
![]() People who want a faster resolution; many disc herniations can improve in 3-6 months on their own, but if pain is too great to wait or deficits appear, surgery is considered.
People who want a faster resolution; many disc herniations can improve in 3-6 months on their own, but if pain is too great to wait or deficits appear, surgery is considered.
In summary, discectomy is for those where the benefits (pain/pressure relief) outweigh the small surgical risk, usually after trying some non-surgical care first (unless urgent).
A neurosurgeon or orthopedic spine surgeon evaluates and ensures the symptoms and imaging match for a good outcome prediction.
What to Expect – Before, During, After
OneTreeHealth
Once you and your surgeon decide on discectomy, you’ll have a pre-op process. This may include routine blood work, possibly stopping certain medications (like blood thinners, certain anti-inflammatories) a week prior.
You’ll get instructions on when to stop eating (usually midnight before if morning surgery). Often, discectomies are done outpatient or with one night hospital stay. On the day, you’ll meet anesthesia team who will plan general anesthesia (you’ll be fully asleep for the procedure).
The surgeon will review procedure and get consent signed. They’ll mark the correct level/side on your skin. You’ll be positioned typically lying face down on a special padded table (for lumbar) or face up if it’s a front-of-neck approach in cervical.
OneTreeHealth
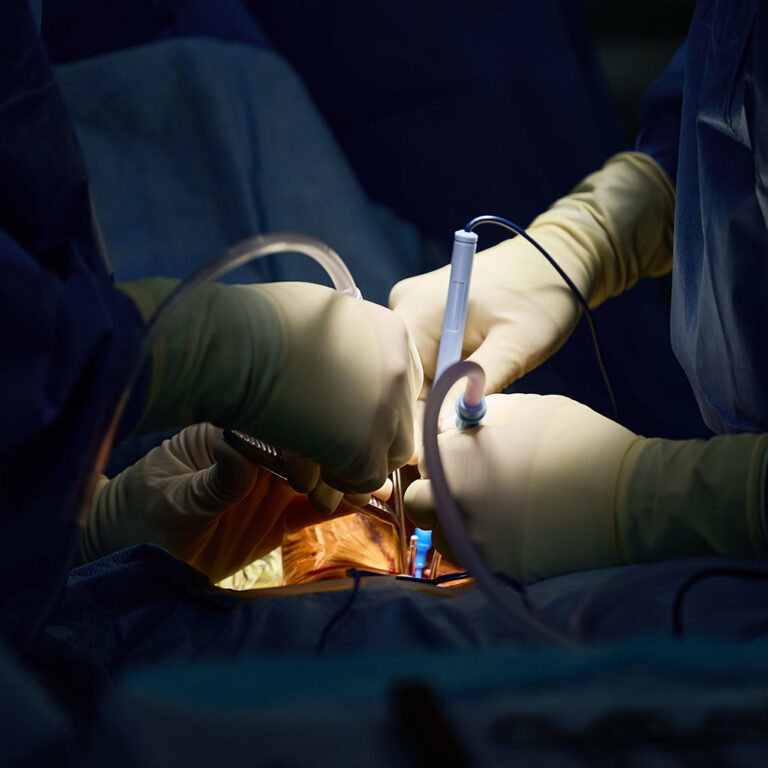
For a lumbar microdiscectomy, after anesthesia, a small incision (often about 1 to 2 inches) is made in the midline of the lower back over the affected level. The muscles are gently separated (not cut through, just moved aside) to expose the bony arch (lamina) of the spine. Sometimes a small bit of bone or ligament is removed (this is called a laminotomy) to create a window to reach the disc. Using operating microscope or magnification, the surgeon identifies the nerve root and gently retracts it to access the disc area. Then the herniated disc fragment is carefully removed using little instruments.
They might remove some loose disc material from inside the disc space to reduce recurrence, but the majority of the disc is left intact. Once the pressure is relieved (the nerve now free), they irrigate, ensure no bleeding (small blood vessels cauterized) and then close the incision – typically with a few dissolvable stitches under the skin and maybe glue or steri-strips outside. The procedure usually takes around 45 minutes to 1 hour for a single level.
For a cervical discectomy, often it’s done from the front (ACDF), meaning a small incision on the front/side of neck, moving aside esophagus, etc., removing disc and usually placing a graft for fusion. That’s a bit different in feel and recovery. But for now, focusing lumbar: minimal blood loss, small incision.

OneTreeHealth
You’ll wake up in recovery. For a microdiscectomy, patients often notice their leg pain is significantly improved immediately! You might have surgical site pain but that terrible shooting sciatic pain is often gone or much less – because the nerve is no longer pinched. You’ll be monitored for a couple of hours. If doing well (able to eat, pee, walk a bit with assistance), many patients go home the same day. Some surgeons keep overnight especially if late in day or if any medical observations needed.
Pain at the incision and muscle area is usually moderate – you’ll get pain meds as needed. You’re encouraged to walk a bit as soon as you’re steady (walking is good for recovery). Limit bending, lifting, twisting for a few weeks to let things heal (commonly, no lifting more than 10-15 lbs for 4-6 weeks). You’ll likely have a follow-up appointment ~2 weeks after to check incision, any neurologic exam, and then later maybe at 6 weeks and a few months to ensure recovery is on track. Many return to light work in 2-4 weeks if it’s sedentary; heavier labor might be 6-8 weeks or more. No driving until off narcotic pain meds and you feel comfortable turning/moving (usually a week or two).
You might be given some back exercises or referred to PT after a few weeks to strengthen core and prevent re-injury. Incision care: keep it dry for first few days, then allow to get lightly wet, pat dry. Watch for any signs of infection (very low chance). We also caution to avoid long sitting for couple weeks – better to get up frequently. You’ll also be instructed on posture and maybe how to log- roll out of bed etc., initially.
Benefits
Benefits include:
<img src="https://www.onetreehealth.com/wp-content/uploads/2025/08/CITYPNG.COMHD-Circle-Green-Tick-Mark-Symbol-Icon-PNG-1500x1500-1-300x300.png" alt="" width="31" height="31" Rapid Relief of Sciatica/ Radicular Pain: Discectomy is one of the most satisfying surgeries in that sense – patients often have almost immediate relief of that awful nerve pain, or at least a large improvement. It addresses the root cause mechanically.
<img src="https://www.onetreehealth.com/wp-content/uploads/2025/08/CITYPNG.COMHD-Circle-Green-Tick-Mark-Symbol-Icon-PNG-1500x1500-1-300x300.png" alt="" width="31" height="31" Minimally Invasive and Quick Recovery: With micro techniques, tissue damage is minimal, so recovery is faster than older style open surgeries. Smaller incision, less pain, and often outpatient.
<img src="https://www.onetreehealth.com/wp-content/uploads/2025/08/CITYPNG.COMHD-Circle-Green-Tick-Mark-Symbol-Icon-PNG-1500x1500-1-300x300.png" alt="" width="31" height="31" High Success Rate: For properly selected cases (single-level disc herniation causing leg pain), success rates for pain relief are quite high, often quoted around 90% for significant relief of leg pain.
<img src="https://www.onetreehealth.com/wp-content/uploads/2025/08/CITYPNG.COMHD-Circle-Green-Tick-Mark-Symbol-Icon-PNG-1500x1500-1-300x300.png" alt="" width="31" height="31" Prevents nerve damage progression: If you had weakness or numbness, removing compression can allow nerves to recover or at least prevent further harm, potentially restoring function over time.
<img src="https://www.onetreehealth.com/wp-content/uploads/2025/08/CITYPNG.COMHD-Circle-Green-Tick-Mark-Symbol-Icon-PNG-1500x1500-1-300x300.png" alt="" width="31" height="31" Improved Quality of Life: Being able to sit, stand, walk, sleep without that constant radiating pain is huge. Many return to normal activities and work fairly soon, which is great.
<img src="https://www.onetreehealth.com/wp-content/uploads/2025/08/CITYPNG.COMHD-Circle-Green-Tick-Mark-Symbol-Icon-PNG-1500x1500-1-300x300.png" alt="" width="31" height="31" Low Risk: It’s considered a safe procedure with a low complication rate in experienced hands.
<img src="https://www.onetreehealth.com/wp-content/uploads/2025/08/CITYPNG.COMHD-Circle-Green-Tick-Mark-Symbol-Icon-PNG-1500x1500-1-300x300.png" alt="" width="31" height="31" It doesn’t significantly alter your anatomy (aside from the bit of disc removed); some disc is left, so you maintain some cushioning. It’s more minor than a fusion because no hardware or fusion of bone is involved, so motion at that level is preserved.
Risks
<img src="https://www.onetreehealth.com/wp-content/uploads/2025/08/CITYPNG.COMHD-Circle-Green-Tick-Mark-Symbol-Icon-PNG-1500x1500-1-300x300.png" alt="" width="31" height="31" Disc Reherniation: Perhaps the biggest risk specifically for discectomy – the same disc can herniate again (either because some fragment was left or another piece extrudes later). Reherniation rates are about 5-10%. If it happens, symptoms could return and sometimes another surgery is needed. We try to minimize by removing loose fragments, but we don’t remove the entire disc (that would destabilize spine), so the disc is still there and could have future issues.
<img src="https://www.onetreehealth.com/wp-content/uploads/2025/08/CITYPNG.COMHD-Circle-Green-Tick-Mark-Symbol-Icon-PNG-1500x1500-1-300x300.png" alt="" width="31" height="31" Infection: As with any surgery – risk is low (<1-2%). Could be superficial (incision infection) or deep (discitis). Precautions (antibiotics during surgery, sterile technique) are taken.
<img src="https://www.onetreehealth.com/wp-content/uploads/2025/08/CITYPNG.COMHD-Circle-Green-Tick-Mark-Symbol-Icon-PNG-1500x1500-1-300x300.png" alt="" width="31" height="31" Dural Tear (CSF leak): The thin covering of the nerves (dura) can sometimes be accidentally nicked or torn, causing spinal fluid leak. Surgeons usually repair it with a stitch or a patch if noticed. It might cause you to have to lay flat a day or two more to heal, and possibly a headache after surgery. Usually manageable, but if not sealed, might need a revision procedure to fix.
<img src="https://www.onetreehealth.com/wp-content/uploads/2025/08/CITYPNG.COMHD-Circle-Green-Tick-Mark-Symbol-Icon-PNG-1500x1500-1-300x300.png" alt="" width="31" height="31" Bleeding: Rarely significant since it’s a small area. But an epidural hematoma (blood clot) can form and if it compresses nerves, might need urgent removal. We monitor post-op for any signs like new severe pain or weakness.
<img src="https://www.onetreehealth.com/wp-content/uploads/2025/08/CITYPNG.COMHD-Circle-Green-Tick-Mark-Symbol-Icon-PNG-1500x1500-1-300x300.png" alt="" width="31" height="31" Nerve Injury: Very low risk, but handling the nerve root carries a slight chance of injury to it or the spinal cord (especially in cervical spine). This could (again rarely) result in worse numbness, weakness or even paralysis if something catastrophic happened. But in the lumbar region, risk of significant nerve damage is extremely small. Minor numbness around the incision or increased numbness in leg (if nerve was very compressed it might be temporarily more irritated when decompressed - that often improves).
<img src="https://www.onetreehealth.com/wp-content/uploads/2025/08/CITYPNG.COMHD-Circle-Green-Tick-Mark-Symbol-Icon-PNG-1500x1500-1-300x300.png" alt="" width="31" height="31" Anesthesia risks: Generic risk of general anesthesia (reaction, breathing issues, etc.), which is low in a short healthy patient surgery.
<img src="https://www.onetreehealth.com/wp-content/uploads/2025/08/CITYPNG.COMHD-Circle-Green-Tick-Mark-Symbol-Icon-PNG-1500x1500-1-300x300.png" alt="" width="31" height="31" Persistent symptoms: In some cases, pain may not fully go away especially if nerve was badly damaged or if there are other issues (like coexisting back pain from arthritis isn’t fixed by discectomy, as it only addresses leg pain). Or there may be scar tissue later that can irritate nerve (epidural fibrosis) – not common but can happen.
<img src="https://www.onetreehealth.com/wp-content/uploads/2025/08/CITYPNG.COMHD-Circle-Green-Tick-Mark-Symbol-Icon-PNG-1500x1500-1-300x300.png" alt="" width="31" height="31" Spinal instability: Removing part of a disc theoretically could contribute to later instability (like a slip or need for fusion later) but for a small disc removal it’s rare. However, if someone has an underlying instability or a very large portion removed, they might later need a fusion. For one-level microdiscectomy, this is not typical.
<img src="https://www.onetreehealth.com/wp-content/uploads/2025/08/CITYPNG.COMHD-Circle-Green-Tick-Mark-Symbol-Icon-PNG-1500x1500-1-300x300.png" alt="" width="31" height="31" Surgeons discuss specific ones based on location – e.g., for cervical discectomy (especially ACDF) they’d mention risks like hoarseness, difficulty swallowing temporarily, etc.
Frequently Asked Questions:
We typically remove only the herniated fragment(s) that are pressing on the nerve, plus any other loose pieces we can easily get to. We don’t remove the entire disc. So yes, most of your disc stays in place and continues to function as a cushion. Imagine the disc like a jelly doughnut – a herniation is some jelly squirting out. We remove that extruded jelly and any that’s obviously about to come out.
But we don’t completely empty the disc because that could cause the disc space to collapse and lead to instability. So you will still have a disc (perhaps slightly thinner because some material is gone). In time, the disc may lose height gradually (as part of degenerative process), but the hope is the nerve won’t be pinched anymore.
Discectomy is most effective for leg pain caused by nerve compression. It may not completely resolve back pain because back pain can come from the disc itself (degenerative changes) or muscles, etc. However, often some back pain that came from muscle spasm or from the disc herniation process might improve once pressure is relieved and you move better. But if your back pain is from generalized arthritis or facet joints, those sources remain.
So, it’s important to clarify: the goal of microdiscectomy is to relieve radicular (nerve) pain and prevent nerve damage. Many patients do experience less overall pain, including back, after recovery, but we cannot guarantee back pain relief to the same degree. If back pain is a dominant symptom, sometimes different approaches are considered (like maybe a fusion if disc space collapsed, etc.). We will discuss with you based on your case.
It depends on what you do and how you heal. For a desk job, some patients return in 1-2 weeks, especially if they can alternate sitting/standing and avoid heavy lifting. It’s wise to give yourself at least one week off, possibly two, to rest and do some walking and allow tissues to start healing. For more physical jobs, you might need to wait 4-6 weeks before heavy lifting or twisting is safe. We usually impose lifting restrictions (~10-15 lbs) for about 4-6 weeks to avoid strain on the healing area. You can do light household tasks within a few days as tolerated, but avoid vacuuming, yard work, etc., for a bit. Gentle walking is actually encouraged right away, increasing gradually. Driving: often okay after 1-2 weeks when you feel comfortable twisting to look around and are off narcotic meds. Light exercise (like stationary bike, or stretching) might be allowed after a couple weeks.
Full sports (like golf, gym workouts) usually after 6-8 weeks with surgeon’s clearance. The key is to listen to your body and your surgeon’s advice. They’ll likely give guidance at follow-ups. Everyone is a bit different, but microdiscectomy tends to have a much faster recovery than bigger surgeries.
If we talk strictly about the same level: as mentioned, roughly 5-10% of patients might experience a recurrent disc herniation at that level at some point. That could be within months or many years later. If that happens, sometimes another discectomy is done; if it recurs multiple times, a fusion might be considered. In general, 90-95% do not need another surgery at that same level, which is good odds.
However, if you have overall degenerative disc disease, other levels could herniate later in life (that’s more related to your spine condition, not caused by the surgery). After one disc herniation, you might be a bit more prone to others because of genetic or wear factors. We advise maintaining a healthy weight, core strength, and good body mechanics to protect your spine long term. If you take care and perhaps do physical therapy post-op for core strengthening, you can reduce the risk of future injuries.
But some factors we can’t control (aging, genetics). So, while another surgery is not likely, it’s not impossible. We’ll of course be there to manage any future issues if they arise.
The scar is usually small – for lumbar, perhaps about an inch or so, vertical line in the lower back. It fades over time to a thin line. It’s placed in a region often covered by clothing or not too conspicuous. Long-term, most people regain full function without limitations after healing. We do advise always being mindful of proper lifting technique and avoid extreme strain to protect your spine in general.
Some patients choose to avoid very high-impact activities to be kind to their back, but generally you can resume normal life, including exercise. The removed disc fragment doesn’t typically “grow back” – though disc can re-herniate as said. The surgery doesn’t make you weaker or anything; after healing, your back muscles recover, and with conditioning, you can be as strong as before. You might have a bit of residual stiffness initially, but most get back to normal flexibility. If nerve damage was present pre-surgery (like numbness or weakness), recovery of that is variable and could take months and sometimes is incomplete. But that’s due to the pre-existing condition, not the surgery itself (the surgery stops further damage and often allows healing, but nerves recover slowly).
The vast majority of patients are happy and go back to their routine, forgetting they even had surgery except for the scar.


Contact Us Today!
Our expert neurosurgeons at One Tree Health can help you find relief with a precise, minimally invasive discectomy.
If you’re suffering from a pinched nerve causing sharp pain, numbness, or weakness in your arm or leg, don’t wait until it gets worse. We’ll carefully evaluate your condition with advanced imaging and exams, and if surgery is right for you, we’ll guide you through every step for a smooth recovery. Experience life without the constant nerve pain – many patients stand up after surgery with a smile, finally free of the agony that’s been holding them back.
Contact One Tree Health’s Neurosurgery team today to discuss your options. Our priority is to protect your nerves and get you back to living fully, as quickly and safely as possible. Don’t let a herniated disc keep you on the sidelines.
Schedule a consultation now and take the first step toward pain relief and getting your life back.
OneTreeHealth provides coordinated, compassionate care for patients recovering from injury specializing in orthopaedics, neurology, surgery, interventional pain management, and more. We simplify the recovery journey by managing care under one roof, so patients can focus on healing.
Useful Links
Reach Us
397 Wallace Rd Nashville, TN 37211 Suite#303
(615) 696-9900
hello@onetreehealth.com
Copyright 2025, One Tree Healthcare. All Rights Reserved.

