Laminectomy
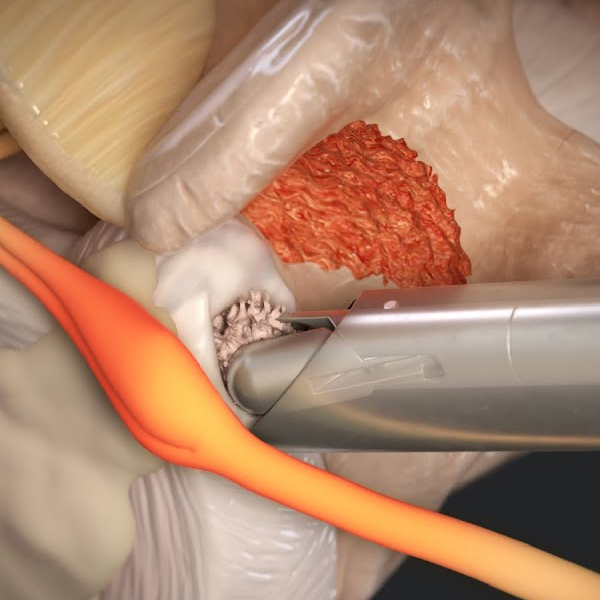
Laminectomy
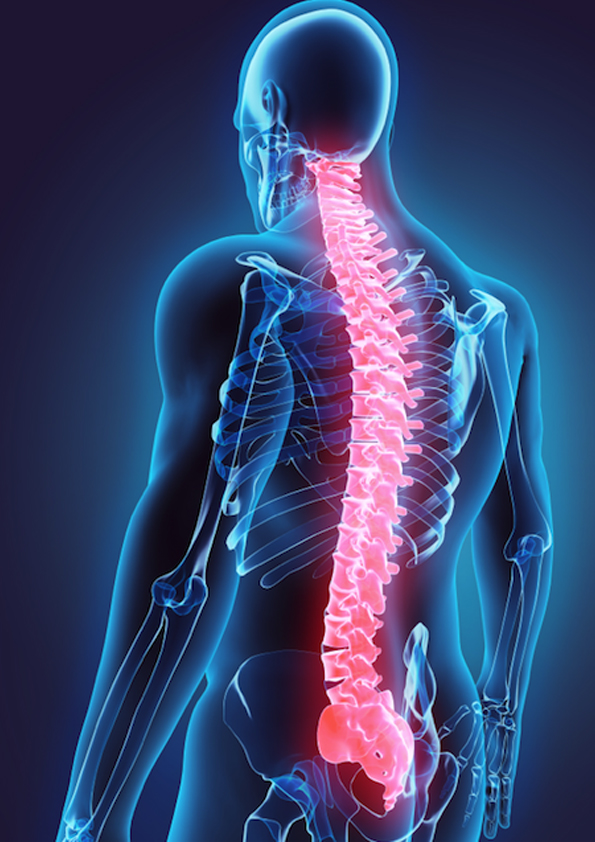
A Laminectomy is a surgical procedure where a portion of the vertebral bone called the lamina (the back part of the vertebra that forms the roof of the spinal canal) is removed to decompress the spinal cord or nerve rootsneurosurgery.columbia.eduhss.edu. Essentially, it creates more space in the spinal canal or nerve passageways (foramina) to relieve pressure. Laminectomy is commonly performed for spinal stenosis, which is a condition where the spinal canal narrows due to arthritis, bone spurs, ligament thickening, or disc bulges, causing compression of the nerves and leading to symptoms like leg pain, numbness, or weakness (especially when standing or walking).
By removing the lamina (and often any thickened ligament or spurs), we enlarge the canal so nerves have breathing room. In the lumbar region, this helps with leg pain and the ability to walk; in the cervical region, it can relieve spinal cord compression and prevent neurological decline. Sometimes laminectomy is combined with other procedures; e.g., a laminectomy plus a fusion if there’s instability. But a “decompression” laminectomy alone often suffices for straightforward stenosis.
Who is it for?
Patients who might need a laminectomy typically have::
![]() Spinal Stenosis (Lumbar): Classic symptoms include neurogenic claudication – pain, cramping, or weakness in the legs brought on by walking/standing and relieved by sitting/bending forward. Imaging (MRI/CT) shows narrowing of the canal and compression of nerve roots (often at multiple levels). If it’s significantly affecting life (can’t walk far, balance issues, etc.) and not responding enough to conservative care (physical therapy, epidural injections, etc.), laminectomy is considered.
Spinal Stenosis (Lumbar): Classic symptoms include neurogenic claudication – pain, cramping, or weakness in the legs brought on by walking/standing and relieved by sitting/bending forward. Imaging (MRI/CT) shows narrowing of the canal and compression of nerve roots (often at multiple levels). If it’s significantly affecting life (can’t walk far, balance issues, etc.) and not responding enough to conservative care (physical therapy, epidural injections, etc.), laminectomy is considered.
![]() Spinal Stenosis (Cervical): If the spinal cord is compressed (cervical stenosis), patients might have hand clumsiness, balance issues, or other myelopathy signs. Laminectomy in the neck (often multiple levels) can free the cord. Usually, a fusion accompanies it in the neck to maintain stability (posterior cervical laminectomy and fusion) unless done selectively with specialized techniques.
Spinal Stenosis (Cervical): If the spinal cord is compressed (cervical stenosis), patients might have hand clumsiness, balance issues, or other myelopathy signs. Laminectomy in the neck (often multiple levels) can free the cord. Usually, a fusion accompanies it in the neck to maintain stability (posterior cervical laminectomy and fusion) unless done selectively with specialized techniques.
![]() Compression from other causes: e.g., a large tumor or a big disc bulge might also require laminectomy to access and remove the offending agent.
Compression from other causes: e.g., a large tumor or a big disc bulge might also require laminectomy to access and remove the offending agent.
![]() Synovial Cysts: Sometimes in lumbar spine, these arthritis-related cysts pinch nerves; removing lamina helps take out the cyst.
Synovial Cysts: Sometimes in lumbar spine, these arthritis-related cysts pinch nerves; removing lamina helps take out the cyst.
![]() People who have tried non-surgical measures and whose symptoms are significant (e.g., severely limited walking, persistent nerve pain, progressing weakness). If there’s any bowel/bladder issues or severe nerve compression signs, surgery is more urgent.
People who have tried non-surgical measures and whose symptoms are significant (e.g., severely limited walking, persistent nerve pain, progressing weakness). If there’s any bowel/bladder issues or severe nerve compression signs, surgery is more urgent.
In summary, if imaging shows nerve crowding and symptoms correlate and are affecting quality of life, a laminectomy is often recommended to prevent further neurological decline and improve symptoms..
What to Expect – Before, During, After
OneTreeHealth
Work-up includes imaging to pinpoint levels (often multiple adjacent levels in lumbar). Possibly an EMG if needed to correlate nerve levels. The surgeon will ensure you’re medically cleared (check heart, etc., if needed). Stop any blood thinners a week prior (to minimize bleed risk). The night before, fast after midnight.
Come in morning of surgery, meet anesthesia (general anesthesia will be used), and sign consent. The surgical plan (levels to decompress) is reviewed. Usually, you’ll be placed face down on the OR table in a supportive frame that relieves pressure on abdomen.
OneTreeHealth
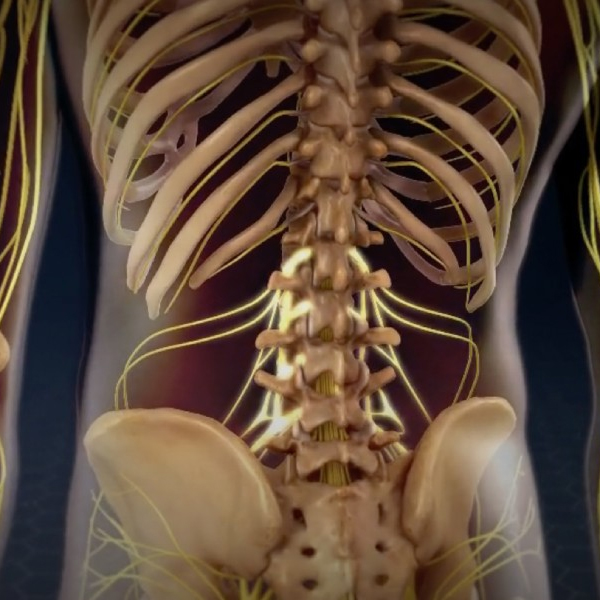
After you’re asleep, an incision is made in the midline over the affected levels. For a multi-level lumbar laminectomy, the incision might be perhaps 2-3 inches or more, depending on levels (e.g., for L3-5, maybe 4 inches). The back muscles (paraspinal muscles) are detached from the lamina on both sides and pulled aside (retracted) to expose the bony arch. Then, using tools like a high-speed burr and rongeurs, the surgeon removes the lamina (right and left) at the target levels, including the spinous process (the bony bump you feel under the skin) as needed.
They also likely remove the thickened ligament (ligamentum flavum) under the lamina, and any bone spurs that are encroaching on nerves. If foraminal stenosis (narrowing where nerve exits), they may perform foraminotomy – shaving bone around the foramen.
The goal is to see the dural sac and nerve roots freely without compression. If it’s just decompression, no hardware is placed typically. However, sometimes if a lot of bone is removed or in presence of instability, they might add screws and rods (fusion) to prevent any post-op instability. But in many pure stenosis cases, especially in older patients, a laminectomy alone is done to maintain mobility. Once decompression is done at all intended levels, they ensure no active bleeding (spine has a lot of small veins; they stop bleeding via cautery or packing). Then they close up: muscles re-attach somewhat, fascia and skin closed with sutures/staples. For a multi-level, surgery might take 1-2 hours, potentially longer if fusion is added.

OneTreeHealth
You’ll wake up in recovery. You’ll have some back pain due to muscle and bone work; medication will be given as needed. Many patients with lumbar laminectomy notice that their leg symptoms improve quickly – standing up, they might have less of that heavy/tingly feeling, as the nerves are free. You will likely stay in the hospital for a day or two, especially if multiple levels or if you need therapy. They’ll get you up and walking the same or next day with assistance. Walking is encouraged (start with short distances, increase gradually).
If no fusion was done, usually you won’t need a brace; if fusion was done, often a brace is provided for a period. Expect incision soreness and stiffness for a few days. You’ll have an incision that needs care – keep it clean and dry, usually covered by a dressing. Stitches or staples often out by 10–14 days. Limit heavy lifting, bending, twisting for a bit (similar restrictions like no >10 lbs for some weeks). But generally, after just laminectomy, surgeons want you to resume gentle activity relatively soon to avoid deconditioning.
Outpatient physical therapy might be recommended after ~4–6 weeks to strengthen back and improve endurance if needed. You might feel immediate improvement in leg endurance or relief of numbness, but if you had a lot of nerve compression, some symptoms (like numbness) can take time to improve, or may not fully resolve if nerve was damaged. Most patients see great improvement in walking ability.
Plan to be off work maybe 4–6 weeks if it’s a physical job, less if it’s desk and you can sit comfortably sooner (maybe 2–3 weeks). Avoid prolonged sitting early on; change positions frequently. We’ll follow up in about 2 weeks, then at 6 weeks, etc., to ensure healing and symptom improvement.
Benefits
Benefits include:
<img src="https://www.onetreehealth.com/wp-content/uploads/2025/08/CITYPNG.COMHD-Circle-Green-Tick-Mark-Symbol-Icon-PNG-1500x1500-1-300x300.png" alt="" width="31" height="31" Improved Mobility and Standing Time: For lumbar stenosis, patients often go from only being able to walk a few minutes or stooping over a cart, to walking much longer distances upright without leg pain or weakness. Quality of life (shopping, traveling) improves dramatically.
<img src="https://www.onetreehealth.com/wp-content/uploads/2025/08/CITYPNG.COMHD-Circle-Green-Tick-Mark-Symbol-Icon-PNG-1500x1500-1-300x300.png" alt="" width="31" height="31" Pain Relief: Leg pain (sciatica-like or cramping) typically lessens significantly. In cervical cases, arm symptoms and even some gait issues can improve. Removing compression can also halt neurological deterioration – critical in cervical myelopathy to maintain function.
<img src="https://www.onetreehealth.com/wp-content/uploads/2025/08/CITYPNG.COMHD-Circle-Green-Tick-Mark-Symbol-Icon-PNG-1500x1500-1-300x300.png" alt="" width="31" height="31" Prevents Falls: If you’re getting weak or numb legs, decompressing nerves can improve strength and sensation, reducing fall risk.
<img src="https://www.onetreehealth.com/wp-content/uploads/2025/08/CITYPNG.COMHD-Circle-Green-Tick-Mark-Symbol-Icon-PNG-1500x1500-1-300x300.png" alt="" width="31" height="31" High Success Rate for Right Indication: For example, lumbar laminectomy for claudication has a success in providing relief to a large majority of patients (studies suggest significant improvement in 80%+ of properly selected patients).
<img src="https://www.onetreehealth.com/wp-content/uploads/2025/08/CITYPNG.COMHD-Circle-Green-Tick-Mark-Symbol-Icon-PNG-1500x1500-1-300x300.png" alt="" width="31" height="31" No Fusion = Maintain Motion: If a laminectomy alone is done, you preserve the natural motion of that segment (unlike a fusion which stops motion). So your flexibility and back movement can remain, just with more space for nerves.
<img src="https://www.onetreehealth.com/wp-content/uploads/2025/08/CITYPNG.COMHD-Circle-Green-Tick-Mark-Symbol-Icon-PNG-1500x1500-1-300x300.png" alt="" width="31" height="31" Relatively Low Risk: While it’s more extensive than a microdiscectomy, it’s still generally safe, especially if just bone removal. The main tasks are mechanical decompression; no messing with organs or major blood vessels in a posterior approach.
<img src="https://www.onetreehealth.com/wp-content/uploads/2025/08/CITYPNG.COMHD-Circle-Green-Tick-Mark-Symbol-Icon-PNG-1500x1500-1-300x300.png" alt="" width="31" height="31" Better Quality of Life: Not only walking, but often sleeping better (no leg aches at night), being able to stand to cook or do hobbies again.
<img src="https://www.onetreehealth.com/wp-content/uploads/2025/08/CITYPNG.COMHD-Circle-Green-Tick-Mark-Symbol-Icon-PNG-1500x1500-1-300x300.png" alt="" width="31" height="31" Protects Spinal Cord (in neck cases): In cervical, you can avoid progression to severe disability by decompressing the cord, which is very important.
Risks
<img src="https://www.onetreehealth.com/wp-content/uploads/2025/08/CITYPNG.COMHD-Circle-Green-Tick-Mark-Symbol-Icon-PNG-1500x1500-1-300x300.png" alt="" width="31" height="31" Injury to Nerves or Cord: Because we are working around the spinal cord/nerves, there’s a risk (albeit low) of injury that could cause neurological deficit (numbness, weakness, or paralysis in worst case). For lumbar, there’s no cord, just nerve roots; injury could cause nerve root damage (e.g., foot drop if L4/L5 nerve severely injured). Surgeons are very careful to avoid this, decompress under direct vision.
<img src="https://www.onetreehealth.com/wp-content/uploads/2025/08/CITYPNG.COMHD-Circle-Green-Tick-Mark-Symbol-Icon-PNG-1500x1500-1-300x300.png" alt="" width="31" height="31" Dural Tear/CSF Leak: Removing lamina and ligament can sometimes nick the dura. If a tear occurs, it’s usually repaired during surgery with a suture or patch, but it might lead to a spinal headache or require some precautions (like lying flat longer). Rarely, if a leak persists, another procedure to fix it might be needed. Risk is a few percent, more if prior surgeries (scar tissue).
<img src="https://www.onetreehealth.com/wp-content/uploads/2025/08/CITYPNG.COMHD-Circle-Green-Tick-Mark-Symbol-Icon-PNG-1500x1500-1-300x300.png" alt="" width="31" height="31" Infection: Could be superficial or deep. Superficial might just need antibiotics; deep could require a washout surgery. Low risk (1-3%). Prevention with antibiotics and sterile technique.
<img src="https://www.onetreehealth.com/wp-content/uploads/2025/08/CITYPNG.COMHD-Circle-Green-Tick-Mark-Symbol-Icon-PNG-1500x1500-1-300x300.png" alt="" width="31" height="31" Bleeding: Laminectomy can sometimes bleed moderately from venous plexus. Usually manageable with surgical techniques. Rarely a significant postoperative hematoma (blood collection) can form and if it compresses nerves, might need urgent re-operation to remove. We watch for severe new pain or neuro deficits post-op as signs.
<img src="https://www.onetreehealth.com/wp-content/uploads/2025/08/CITYPNG.COMHD-Circle-Green-Tick-Mark-Symbol-Icon-PNG-1500x1500-1-300x300.png" alt="" width="31" height="31" Incomplete Relief: If some compression wasn’t fully addressed (e.g., far lateral stenosis not adequately decompressed) or if neuropathy was already advanced, some symptoms might persist. Also, laminectomy addresses nerve compression but not back pain from arthritis – so you might still have some back ache from facets or muscular, though often improved due to increased activity ability.
<img src="https://www.onetreehealth.com/wp-content/uploads/2025/08/CITYPNG.COMHD-Circle-Green-Tick-Mark-Symbol-Icon-PNG-1500x1500-1-300x300.png" alt="" width="31" height="31" Scar Tissue: After any spine surgery, scar tissue forms and could potentially tether nerve roots, causing some residual symptoms (epidural fibrosis). There’s not a lot to do to prevent that aside from meticulous technique; usually it’s not symptomatic but occasionally can contribute to persistent pain.
<img src="https://www.onetreehealth.com/wp-content/uploads/2025/08/CITYPNG.COMHD-Circle-Green-Tick-Mark-Symbol-Icon-PNG-1500x1500-1-300x300.png" alt="" width="31" height="31" General Risks: Anesthesia risk, blood clots in legs (less common than in bigger surgeries but prophylaxis measures taken if patient at risk), etc.
Frequently Asked Questions:
Incision size depends on how many levels we do. For one level, it could be ~2 inches; for multiple, 3–5 inches potentially. We try to minimize it but also need enough exposure to work safely.
Regarding fusion: if you have evidence of instability (like a slipped vertebra or a lot of facet joint removal is needed), the surgeon might recommend doing a fusion with screws and rods to stabilize and prevent future issues. If your spine is stable and we can preserve enough of the facet joints, we often do not fuse. It’s case-by-case.
Without fusion, recovery is a bit quicker and you keep motion. Surgeons aim to avoid fusion if possible for isolated stenosis, especially in older patients, to reduce surgery magnitude. But if needed (for example, if you have a slip at L4–5 causing stenosis), then a fusion might be done concurrently.
We’ll review your imaging beforehand and discuss if fusion is on the table or not.
Many patients notice improvement immediately in certain aspects – e.g., they stand up the day after surgery and realize the heaviness or pain in the calves is much less. For others, it may be gradual as inflammation subsides.
Generally, within days to weeks, you should see significant changes: you can walk further without needing to sit, or numbness/tingling improves. If there was weakness, that might take weeks to months to recover strength, depending on nerve healing.
In cervical cases, sometimes improvements in dexterity and gait are noticed within weeks, but if damage was long-standing, some things might not reverse fully (the goal was to stop it from getting worse and hopefully regain some function).
Pain often gets better pretty fast – the classic leg pains of stenosis ease up. You will have surgical pain for a week or two, but that’s manageable and temporary. After that, you may feel just soreness if you overdo it.
Each patient is different, but by 6 weeks, we expect you to be doing a lot more than pre-surgery, with less pain.
Laminectomy is primarily aimed at nerve compression (leg symptoms for lumbar, etc.). It doesn’t directly address back pain caused by arthritis or disc degeneration. Some patients find their back feels better because they can be more active and the removal of bony pressure relieves some achiness.
But it’s possible to still have some back pain post-op, as the underlying arthritis is still there (we just removed bone to relieve nerves). We will work on managing any residual back pain with therapy, exercise, and possibly medications.
If your back pain was largely muscular due to limited mobility, it might improve when you walk more. But if it’s facet arthritis, you might still feel stiffness or ache. That’s where physical therapy and core strengthening later can help.
We set expectations that the goal is nerve pain relief and improved walking, not necessarily a cure-all for any back ache. However, improved function can indirectly reduce some back pain in the long run.
Initially, we usually advise caution for about 6 weeks: avoid heavy lifting, bending, or twisting your spine a lot. This allows muscles and tissues to heal. After that, you gradually resume normal activities, guided by how you feel and possibly therapy. We encourage staying active but using good body mechanics.
As for stenosis returning: the bone we removed is gone for good (it doesn’t regrow significantly). However, degenerative changes can continue – other levels might develop stenosis over time. Or if only a partial laminectomy was done at a certain level, more spurs could form later. But generally, the decompressed levels stay decompressed.
The aging process continues, so say 10 years down the road, another level could narrow and cause symptoms. If one segment is freed and adjacent segments were borderline, sometimes patients can develop new symptoms from those later. Also, if no fusion was done and later instability occurs, that could cause a need for further surgery in the future.
But in many cases, a laminectomy gives lasting relief for that level’s issue. We’ll monitor your spine health on follow-ups. Maintaining a healthy lifestyle (weight control, core strength) can slow degeneration. There’s no guarantee stenosis won’t affect other parts of your spine eventually, but we address issues as they arise.
Yes, likely after the initial healing period. In the hospital, you’ll get basic instruction on walking and gentle movements. Once your incision is healed and you’re 4–6 weeks out, we often prescribe outpatient physical therapy.
The focus will be on strengthening your core and back muscles, improving flexibility, and practicing safe movement patterns. Therapy can also help you rebuild endurance for walking and teach balance exercises if needed (especially for those who had gait issues before).
It’s not mandatory in every case; some patients do fine with just home exercises and a walking regimen. But many benefit from guided PT to speed recovery and address any muscle weakness that developed while you were limited pre-op.
We definitely encourage daily walking as the best exercise starting soon after surgery (with increasing distance as tolerated). Swimming (once the incision is healed) or water therapy is great too, down the line.
The goal is to get you back to normal activity, so PT is a tool to help achieve that and possibly reduce any persistent low back stiffness. We’ll tailor recommendations to your age, condition, and personal goals.

Contact Us Today!
Don’t let spinal stenosis or nerve compression keep you from living an active life.
At One Tree Health, our skilled neurosurgeons specialize in laminectomy procedures that can free up those pinched nerves and get you moving comfortably again.
If you’re struggling with leg pain, numbness, or weakness that limits your walking—or signs of spinal cord pressure—we’re here to help. We’ll perform a thorough evaluation and walk you through the best treatment options. If surgery is needed, you can trust our team to use the latest techniques to ensure a safe procedure and a smooth recovery.
Many of our patients are back to enjoying daily walks, hobbies, and time with family without the pain that once held them back.
Take the first step toward relief – contact One Tree Health’s Neurosurgery department to schedule a consultation. We’re committed to getting you back on your feet, standing tall and pain-free.
You don’t have to accept the limitations of spinal stenosis. Let’s open up those channels and give your nerves the breathing room they need. Call us today and find out how we can help improve your quality of life with expert spinal care.
OneTreeHealth provides coordinated, compassionate care for patients recovering from injury specializing in orthopaedics, neurology, surgery, interventional pain management, and more. We simplify the recovery journey by managing care under one roof, so patients can focus on healing.
Useful Links
Reach Us
397 Wallace Rd Nashville, TN 37211 Suite#303
(615) 696-9900
hello@onetreehealth.com
Copyright 2025, One Tree Healthcare. All Rights Reserved.

