Spinal Cord Stimulators
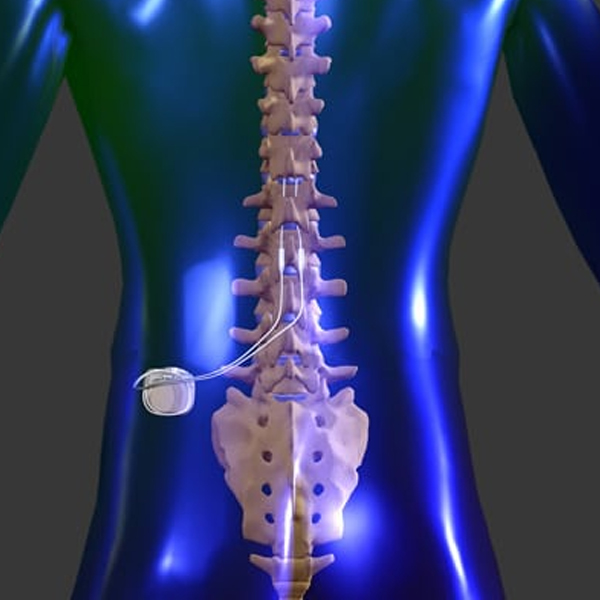
What is a Spinal Cord Stimulator (SCS)?
A Spinal Cord Stimulator is an implanted medical device that uses mild electrical pulses to interrupt pain signals along the spinal cord. It’s like a “pacemaker for pain.” The device system has thin wires (electrodes) placed in the epidural space near the spinal cord and a small battery-powered generator (like a pacemaker) implanted under the skin (typically in the buttock or abdomen). The electrical impulses it generates modulate the nerves’ activity so that pain is not perceived as intensely. Instead of pain, patients might feel a gentle tingling or no sensation at all. SCS doesn’t fix the source of pain, but it changes how your brain perceives it, offering significant relief for many with chronic pain conditions that haven’t responded to other treatments.
Who is it for?
SCS is usually considered for patients with chronic, severe pain who have tried and exhausted other conservative and interventional treatments. Common indications
include:
Situations include:
![]() Failed Back Surgery Syndrome (FBSS): patients who have persistent back and leg pain even after spine surgeries (like laminectomies or fusions). SCS can help manage what’s also termed post-laminectomy syndrome.
Failed Back Surgery Syndrome (FBSS): patients who have persistent back and leg pain even after spine surgeries (like laminectomies or fusions). SCS can help manage what’s also termed post-laminectomy syndrome.
![]() Complex Regional Pain Syndrome (CRPS): severe nerve pain in a limb after an injury or surgery that hasn’t improved with other measures.
Complex Regional Pain Syndrome (CRPS): severe nerve pain in a limb after an injury or surgery that hasn’t improved with other measures.
![]() Peripheral Neuropathy pain: in some cases of refractory diabetic neuropathy or other neuropathic pain where meds aren’t enough.
Peripheral Neuropathy pain: in some cases of refractory diabetic neuropathy or other neuropathic pain where meds aren’t enough.
![]() Chronic nerve pain: e.g., chronic sciatic pain or radiculopathy that can’t be surgically resolved or patient isn’t surgical candidate.
Chronic nerve pain: e.g., chronic sciatic pain or radiculopathy that can’t be surgically resolved or patient isn’t surgical candidate.
![]() Angina or Peripheral Vascular Disease pain: Rarely used nowadays, but SCS has been used to treat intractable chest pain from heart disease or leg pain from arterial disease, by improving blood flow and blocking pain.
Angina or Peripheral Vascular Disease pain: Rarely used nowadays, but SCS has been used to treat intractable chest pain from heart disease or leg pain from arterial disease, by improving blood flow and blocking pain.
![]() Arachnoiditis or spinal cord injury pain: severe constant pain from these conditions might respond. Essentially, if you have pain primarily in the limbs or trunk due to nerve-related issues and nothing else has provided adequate relief, SCS could be an option. Patients typically have undergone things like physical therapy, medications, injections, maybe surgeries. SCS is a more advanced step, so we ensure you’ve had a thorough workup and that it’s neuropathic-type pain (nerve pain) which responds best to SCS.
Arachnoiditis or spinal cord injury pain: severe constant pain from these conditions might respond. Essentially, if you have pain primarily in the limbs or trunk due to nerve-related issues and nothing else has provided adequate relief, SCS could be an option. Patients typically have undergone things like physical therapy, medications, injections, maybe surgeries. SCS is a more advanced step, so we ensure you’ve had a thorough workup and that it’s neuropathic-type pain (nerve pain) which responds best to SCS.
Important: SCS Trial – Before committing to a permanent implant, patients undergo a trial: temporary electrodes are placed and connected to an external stimulator for about a week. If you get at least 50% pain reduction and improved function during the trial, we consider it successful and proceed to permanent implant. If not, the trial leads are removed and we don’t implant.
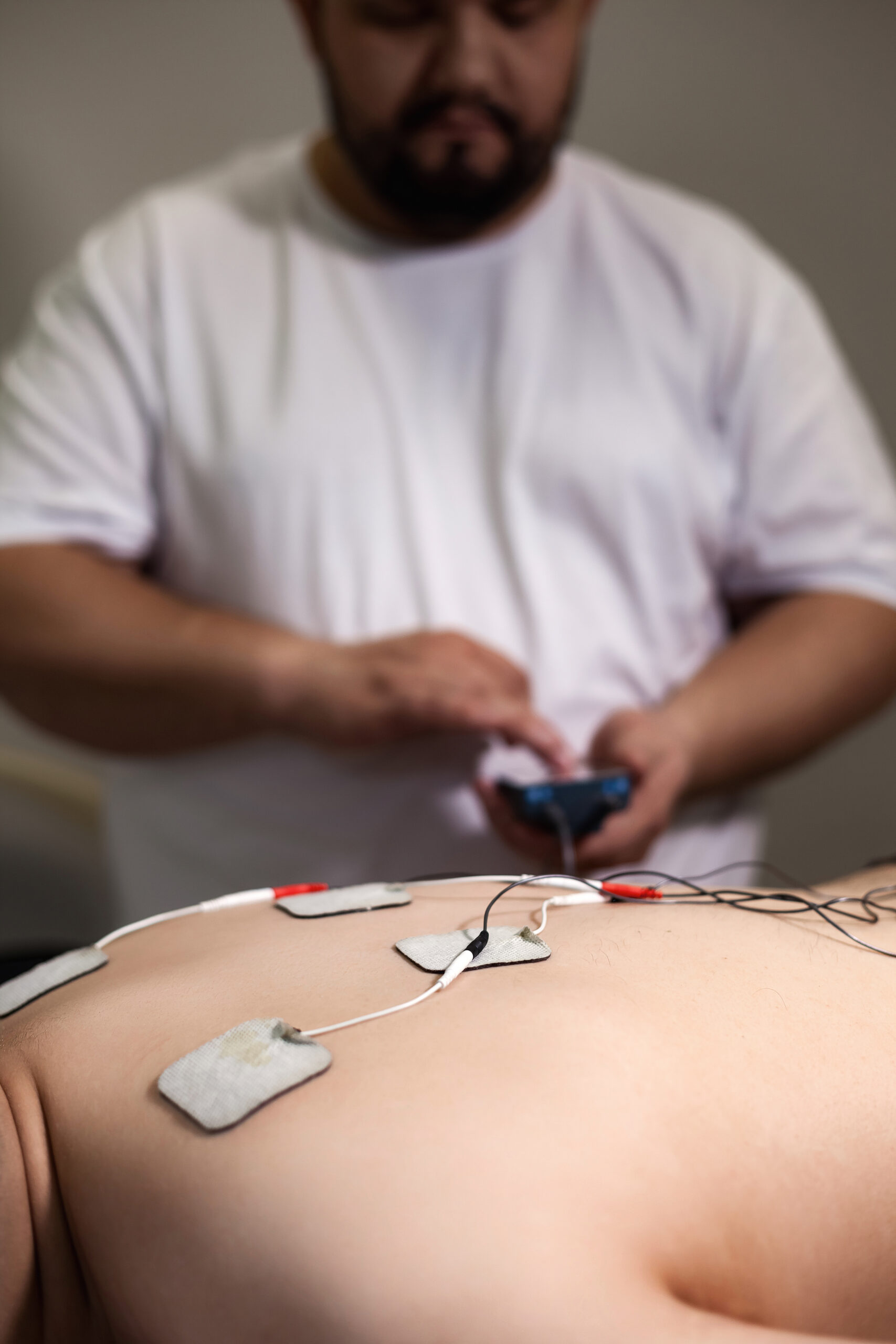
What to Expect – Trial and Permanent Implant
OneTreeHealth
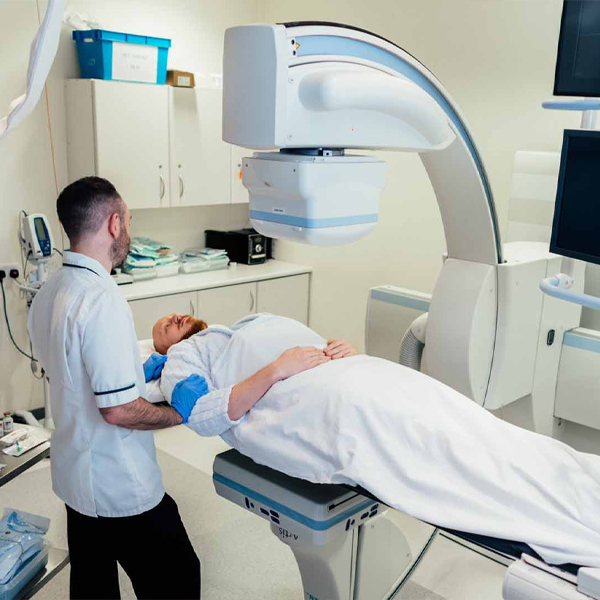
The trial is usually an outpatient procedure under local anesthesia (with maybe mild sedation). We use fluoroscopy to insert one or two thin leads through a needle into your epidural space (similar entry as an epidural injection). We position the leads ideally at the level corresponding to your pain distribution (e.g., mid back for leg pain). You’ll be awake enough to give feedback; we test the stimulator with an external device and ask if you feel tingling in the painful areas.
Once positioned and you feel coverage, we secure the leads to skin with dressings. The leads exit the skin and attach to a small external battery that you wear on a belt. We program some initial settings. You go home that day with instructions to use the stimulator over the next 5-7 days. You should avoid vigorous movement (so the leads don’t move) – no bending, twisting, raising arms high, etc. Keep the area dry. During the trial, you note your pain levels and how much relief and any issues.
We’ll follow up or have you keep a diary. After the trial period, we remove the leads in clinic (just gently pull them out – takes seconds, since they aren’t anchored).
OneTreeHealth
If trial was successful (usually defined by ≥50% pain relief and the patient is happy with the result), we plan for permanent implant. If not, we unfortunately tell you SCS might not be right for you and explore other options.
OneTreeHealth
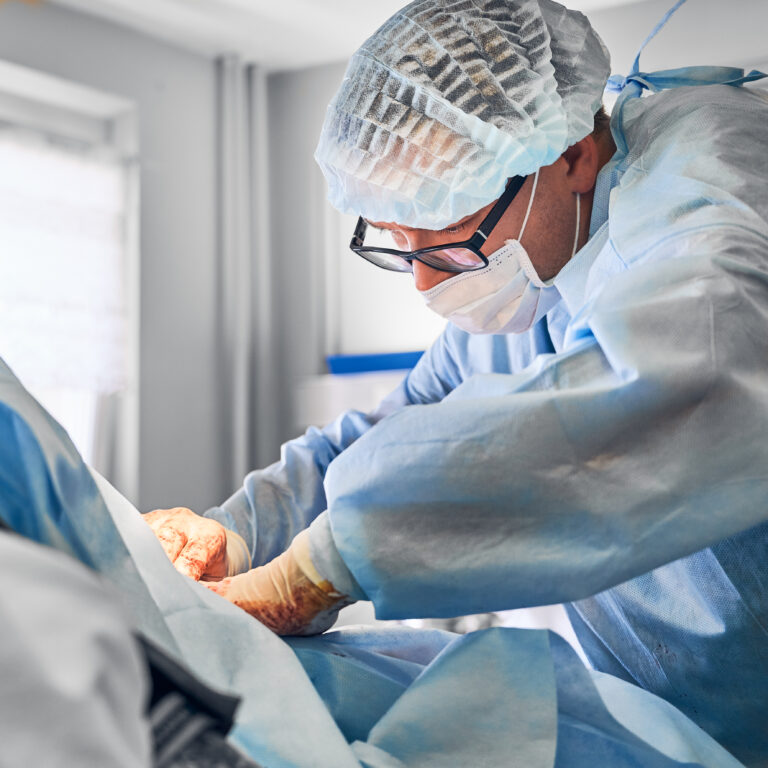
This is done in the operating room, often under conscious sedation or general anesthesia depending. It’s still usually outpatient or one-night stay. Similar to trial, leads are placed in epidural space but now we secure them (sometimes leads have small anchors or we suture them to a ligament so they don’t move).
Then we create a small pocket under the skin (commonly in the upper buttock or low flank) for the generator (a device about the size of a silver dollar but thicker). We tunnel the lead wires under the skin to connect to the generator. Once all is in place, we test the system again before closing incisions.
You’ll have 1-2 incisions (one midline back ~2 inches long for leads, one on the buttock ~2-3 inches for generator). These are closed with stitches or staples.

OneTreeHealth
You may have some post-surgical soreness in your back and buttock from the incisions – that’s normal. We’ll give wound care instructions and limited activity instructions (no heavy lifting, twisting for ~6-8 weeks to let leads scar in place). The stimulator will be active and we’ll have an initial program set, but we’ll fine-tune it in follow-up visits.
You’ll also get a handheld remote to adjust the strength (and sometimes switch programs for different positions or activities). Modern stimulators even have options for “paraesthesia-free” stimulation (meaning you don’t feel tingling, just pain relief). Over a few sessions, our team will optimize the programming to give you the best pain control in various situations (e.g., a program for when you’re lying, another for active, etc.). Battery: some devices are rechargeable (you have to charge it through the skin every week or so), others are non-rechargeable and last a few years then need replacing. We’ll pick based on your preferences and usage.
You’ll carry an ID card that you have an implant (important for MRIs – some newer devices are MRI-compatible under certain conditions). We follow up regularly to manage pain and any device issues.
Benefits
SCS can significantly improve quality of life for those with otherwise untreatable pain. Benefits include:
<img src="https://www.onetreehealth.com/wp-content/uploads/2025/08/CITYPNG.COMHD-Circle-Green-Tick-Mark-Symbol-Icon-PNG-1500x1500-1-300x300.png" alt="" width="31" height="31" Significant Pain Reduction: Many patients achieve 50-70% less pain. Some even more. This can mean going from bedridden to active again.
<img src="https://www.onetreehealth.com/wp-content/uploads/2025/08/CITYPNG.COMHD-Circle-Green-Tick-Mark-Symbol-Icon-PNG-1500x1500-1-300x300.png" alt="" width="31" height="31" Reduced Medication Use: With pain relief, many can decrease or stop heavy pain meds (like opioids), which is better for their overall health and avoids side effects.
<img src="https://www.onetreehealth.com/wp-content/uploads/2025/08/CITYPNG.COMHD-Circle-Green-Tick-Mark-Symbol-Icon-PNG-1500x1500-1-300x300.png" alt="" width="31" height="31" Better Function: Patients often report they can walk farther, sleep better, and do daily tasks they couldn’t before.
<img src="https://www.onetreehealth.com/wp-content/uploads/2025/08/CITYPNG.COMHD-Circle-Green-Tick-Mark-Symbol-Icon-PNG-1500x1500-1-300x300.png" alt="" width="31" height="31" Reversible & Adjustable: Unlike a one-time surgery, SCS is adjustable – if pain patterns change, we can reprogram it. If you ever decide you don’t want it or it’s not helping, it can be turned off or removed.
<img src="https://www.onetreehealth.com/wp-content/uploads/2025/08/CITYPNG.COMHD-Circle-Green-Tick-Mark-Symbol-Icon-PNG-1500x1500-1-300x300.png" alt="" width="31" height="31" Avoids Major Surgery: It’s a less invasive approach compared to something like redoing spine surgery, cutting nerves, etc. It doesn’t damage nerves; it just modulates them. If new treatments or surgeries come up later, SCS can be
removed to pursue those.
<img src="https://www.onetreehealth.com/wp-content/uploads/2025/08/CITYPNG.COMHD-Circle-Green-Tick-Mark-Symbol-Icon-PNG-1500x1500-1-300x300.png" alt="" width="31" height="31" Improved Mood and Sleep: Chronic pain often leads to depression and insomnia. By alleviating pain, mood and sleep often improve.
<img src="https://www.onetreehealth.com/wp-content/uploads/2025/08/CITYPNG.COMHD-Circle-Green-Tick-Mark-Symbol-Icon-PNG-1500x1500-1-300x300.png" alt="" width="31" height="31" For certain conditions (like CRPS), SCS is one of the only effective treatments to regain limb use and reduce extreme pain..
Risks
SCS implantation is a surgical procedure, so it carries risks:
<img src="https://www.onetreehealth.com/wp-content/uploads/2025/08/CITYPNG.COMHD-Circle-Green-Tick-Mark-Symbol-Icon-PNG-1500x1500-1-300x300.png" alt="" width="31" height="31" Infection: There’s a risk of infection at the implant site or along the leads (reported in a small percentage of cases). This can be serious, as it might require removing the device to clear the infection.
<img src="https://www.onetreehealth.com/wp-content/uploads/2025/08/CITYPNG.COMHD-Circle-Green-Tick-Mark-Symbol-Icon-PNG-1500x1500-1-300x300.png" alt="" width="31" height="31" Lead Movement or Failure: Leads can migrate (move slightly) or the device can malfunction. If a lead moves, stimulation might no longer cover the pain area (pain returns or you feel it somewhere else). Revision surgery might be needed to reposition a lead. Devices can rarely fail or battery issues can arise (they are electronics after all).
<img src="https://www.onetreehealth.com/wp-content/uploads/2025/08/CITYPNG.COMHD-Circle-Green-Tick-Mark-Symbol-Icon-PNG-1500x1500-1-300x300.png" alt="" width="31" height="31" Dural Puncture: While placing leads, accidental spinal fluid leak could occur (dural puncture) causing headache. We try to avoid this by technique (the epidural space, not piercing the dura).
<img src="https://www.onetreehealth.com/wp-content/uploads/2025/08/CITYPNG.COMHD-Circle-Green-Tick-Mark-Symbol-Icon-PNG-1500x1500-1-300x300.png" alt="" width="31" height="31" Pain at Implant Site: Some people experience persistent discomfort at the generator pocket site or along the lead track. Often it fades, but in some cases the hardware can be annoying (thin patients might feel the implant more).
<img src="https://www.onetreehealth.com/wp-content/uploads/2025/08/CITYPNG.COMHD-Circle-Green-Tick-Mark-Symbol-Icon-PNG-1500x1500-1-300x300.png" alt="" width="31" height="31" Nerve Damage: Extremely rare, but there is a slight risk during lead placement of nerve injury, which could potentially cause neurological deficits. We’re very careful and use live imaging to avoid this.
<img src="https://www.onetreehealth.com/wp-content/uploads/2025/08/CITYPNG.COMHD-Circle-Green-Tick-Mark-Symbol-Icon-PNG-1500x1500-1-300x300.png" alt="" width="31" height="31" Loss of Efficacy Over Time: Sometimes, even if it works initially, scar tissue or nerve changes might reduce effectiveness over years.
<img src="https://www.onetreehealth.com/wp-content/uploads/2025/08/CITYPNG.COMHD-Circle-Green-Tick-Mark-Symbol-Icon-PNG-1500x1500-1-300x300.png" alt="" width="31" height="31" Specific complications: If stimulating cervical spine, rarely can trigger headaches if mis-positioned. Stimulating too high could affect blood pressure or muscle control (so we don’t do that).
<img src="https://www.onetreehealth.com/wp-content/uploads/2025/08/CITYPNG.COMHD-Circle-Green-Tick-Mark-Symbol-Icon-PNG-1500x1500-1-300x300.png" alt="" width="31" height="31" MRI issues: If you have an older or non MRI-compatible device, MRIs can be contraindicated (or require special protocols). We consider this in patient selection (we’d usually use MRI-compatible systems nowadays).
<img src="https://www.onetreehealth.com/wp-content/uploads/2025/08/CITYPNG.COMHD-Circle-Green-Tick-Mark-Symbol-Icon-PNG-1500x1500-1-300x300.png" alt="" width="31" height="31" Cost and Maintenance: SCS is expensive, though insurance often covers it for appropriate cases. The device battery will eventually need replacement (more surgery, albeit minor), usually in 5-10 years or if earlier if non-rechargeable. Rechargeable ones can last longer but you have to charge them regularly.
Overall, nerve blocks are low-risk when done carefully, but we always tailor the approach to the patient’s anatomy and needs. We discuss any specific risk that might apply to the nerve we’re blocking ahead of time.
Frequently Asked Questions:
It depends on programming. Traditional SCS creates a mild tingling/buzzing sensation (paresthesia) in the area of pain, which overlaps and “distracts” from the pain. You typically feel that instead of pain. Many patients get used to it and don’t find it unpleasant – some even find it soothing. Newer “high-frequency” or “burst” stimulation can be programmed so that you don’t consciously feel any tingling (paresthesia-free); the pain just reduces.
We can try different modes. You’ll have a remote to adjust intensity if needed (e.g., you might turn it up when active, down when resting). It should never deliver a shock or anything; if you feel something uncomfortable, we adjust the programming. We always instruct: don’t drive a car while adjusting or if stimulation could be distracting until stable settings are found – but most can drive fine once they’re used to it.
Yes, you can travel and use normal electronics. Airport metal detectors may pick up the metal in the device; you will have an ID card to show security. Usually, you’ll request a pat-down instead of going through the metal detector or full-body scanner, to be safe.
Handheld security wands can interfere if directly over the device, so it’s best to avoid those near it as well. As for phones and appliances, they generally do not interfere. Very strong electromagnetic fields (like certain industrial equipment or MRI machines) can, which is why MRI is a consideration. But everyday things like microwaves, cell phones, radios are fine. Just keep your stimulation remote and charger away from strong magnets. And don’t put cell phone right next to the implant for long periods (like a pocket over it) to be extra cautious, though it’s usually fine.
It’s rare to be 100% pain-free, but many patients experience a dramatic reduction. The goal we set is usually at least 50% reduction in pain intensity. Some do report 80-100% relief, but we don’t promise that. We also aim to improve functional abilities – maybe you can stand an hour instead of 5 minutes, or sleep through the night, etc. You might still have to manage some residual pain with occasional meds or therapy, but it should be much more tolerable.
Think of SCS as a tool to manage chronic pain when other tools have failed. It’s quite successful when properly used, but it’s not an absolute cure for the underlying condition (e.g., it won’t remove arthritis or heal nerve damage, just mask the pain from it). We also encourage continuing a healthy lifestyle, exercise, etc., as tolerated, to maximize overall well-being.
If you have a rechargeable battery (which many newer ones are), you might need to recharge it about once a week (some devices maybe 1-2 times per month, depending on usage and programming intensity). Charging is done wirelessly by placing a charger paddle on your skin over the device for an hour or two. We instruct you fully; it becomes routine, like charging your phone. If you choose a non-rechargeable battery (maybe to avoid dealing with charging), those are sealed units that typically last 3-5 years on average (shorter if you use high settings often). When depleted, you’d need a minor surgery (incision over the generator site) to replace the battery unit. It’s a simpler procedure than initial implant (leads stay in place). We’ll discuss pros/cons of each type. Many prefer rechargeable to avoid frequent replacements, especially if younger.
Generally yes, but always inform healthcare providers you have an SCS. MRI compatibility depends on device type – many are now labeled “MRI Conditional,” meaning you can get an MRI under certain guidelines (like using specific machine settings, etc.).
If MRI is needed for an emergency and your device isn’t compatible, the device may need to be turned off or rarely removed – but we plan ahead if MRI is foreseeable. CT scans, X-rays, and ultrasounds are fine (the device might cause artifact on images in that area, keep in mind).
You should avoid diathermy (a type of deep heat therapy) as it can interact dangerously. If you need surgery in the area of the leads or device, the surgeon needs to be aware so they don’t disturb it. Dental work is fine (some caution with electrocautery if you have device on – usually just turn it off for surgeries). We give you a booklet with all these do’s and don’ts.



Contact Us Today!
Spinal Cord Stimulator might be the solution you’ve been waiting for.
At One Tree Health, we have the expertise to determine if you’re a good candidate and to guide you through a trial of this advanced therapy. Many patients regain control of their lives thanks to SCS – experiencing dramatic pain reduction and improvements in daily function. You don’t have to accept a life of pain.
Contact our pain management team today to explore whether spinal cord stimulation can help you. We’ll provide a thorough evaluation, answer all your questions, and if appropriate, set up a no-risk trial so you can feel the difference for yourself. Take the next step towards a more comfortable, active life.
Schedule an appointment with One Tree Health’s specialists and open the door to long-term pain relief with spinal cord stimulation therapy.
OneTreeHealth provides coordinated, compassionate care for patients recovering from injury specializing in orthopaedics, neurology, surgery, interventional pain management, and more. We simplify the recovery journey by managing care under one roof, so patients can focus on healing.
Useful Links
Reach Us
397 Wallace Rd Nashville, TN 37211 Suite#303
(615) 696-9900
hello@onetreehealth.com
Copyright 2025, One Tree Healthcare. All Rights Reserved.

