Spinal Fusion
What is a Spinal Fusion?
A Spinal Fusion is a surgery designed to permanently join two or more vertebrae together, eliminating motion at that segment. This is achieved by placing bone graft between the vertebrae and often using hardware (such as screws, rods, or plates) to hold the spine in the correct position while the bone heals (fuses).
Over time, the bone graft grows and connects the vertebrae, much like how a broken bone heals—except here we intend the bones to heal as one solid piece.
Fusions can be done in any part of the spine – cervical, thoracic, lumbar – depending on the condition. There are different approaches (from the front, back, side) and techniques (with cages, etc.), but the end goal is the same: stabilize the spine by eliminating movement at a painful or unstable segment.
Who is it for?
Spinal fusion is typically recommended for:
![]() Spinal Instability: For example, spondylolisthesis (one vertebra slipping forward over another) that causes pain or nerve compression. Fusing stops the slip from moving.
Spinal Instability: For example, spondylolisthesis (one vertebra slipping forward over another) that causes pain or nerve compression. Fusing stops the slip from moving.
![]() Severe Degenerative Disc Disease or Chronic Low Back Pain from a Specific Level: If one disc is severely degenerated and causing a lot of pain and other treatments fail, fusion of that level might reduce pain by stopping painful motion.
Severe Degenerative Disc Disease or Chronic Low Back Pain from a Specific Level: If one disc is severely degenerated and causing a lot of pain and other treatments fail, fusion of that level might reduce pain by stopping painful motion.
![]() Recurrent Disc Herniations: After multiple discectomy surgeries at the same level or if the disc space is severely collapsed, a fusion may be done to solve the issue.
Recurrent Disc Herniations: After multiple discectomy surgeries at the same level or if the disc space is severely collapsed, a fusion may be done to solve the issue.
![]() Spinal Deformities: Scoliosis or kyphosis – fusions are done to correct and solidify the curvature.
Spinal Deformities: Scoliosis or kyphosis – fusions are done to correct and solidify the curvature.
![]() Trauma: Fractures that make the spine unstable often require fusion (with screws/rods) to allow healing in proper alignment.
Trauma: Fractures that make the spine unstable often require fusion (with screws/rods) to allow healing in proper alignment.
![]() Neck Issues: For instance, a two-level discectomy in the neck often is accompanied by fusion (ACDF) with a plate to maintain disc height and relieve cord pressure.
Neck Issues: For instance, a two-level discectomy in the neck often is accompanied by fusion (ACDF) with a plate to maintain disc height and relieve cord pressure.
![]() Tumor or Infection Surgeries: If a vertebra is removed or unstable due to these, fusion hardware helps reconstruct stability.
Tumor or Infection Surgeries: If a vertebra is removed or unstable due to these, fusion hardware helps reconstruct stability.
![]() Also, sometimes as part of stenosis surgery: For example, if a lot of bone is removed and facets are compromised, adding a fusion at that level can prevent post-op instability.
Also, sometimes as part of stenosis surgery: For example, if a lot of bone is removed and facets are compromised, adding a fusion at that level can prevent post-op instability.
It’s usually considered when conservative measures (medications, therapy, injections) haven’t helped or aren’t appropriate, and when the cause of pain or problem is well-localized. Because fusion is a bigger deal (as it permanently changes your spine’s motion), surgeons carefully evaluate that it’s necessary and likely to benefit the patient.
What to Expect – Before, During, After
OneTreeHealth
Work-up may include X-rays in flexion/extension (to see instability), CT, and MRI. You’ll discuss with the surgeon which levels to fuse and the approach (anterior vs. posterior, etc.).
Stop smoking if you smoke – this is important because smoking hinders bone healing (fusion success). You may also be advised to take calcium and vitamin D to optimize bone health. Stop blood thinners if you’re on any. Pre-op clearance by your primary doctor may be needed.
On the day of surgery, you’ll undergo general anesthesia. Depending on the approach, you might be positioned on your back (for anterior approach like ALIF or ACDF) or on your stomach (for posterior approach such as PLIF or TLIF). Sometimes both approaches are used—either staged or combined (anterior then posterior).
It’s a more extensive surgery, typically taking a few hours.
OneTreeHealth
Let’s consider a common example: Posterior Lumbar Fusion (with instrumentation).
After anesthesia, an incision is made in the midline back over the levels to fuse (maybe 3–6 inches long depending on how many levels). Muscles are retracted off the spine to expose the bone.
First, any decompression needed is done (like a laminectomy if needed for nerves). Then the surgeon prepares the fusion: they may remove the remaining disc material (if doing an interbody fusion) or decorticate bone surfaces (scrape them to bleeding bone) to place bone graft.
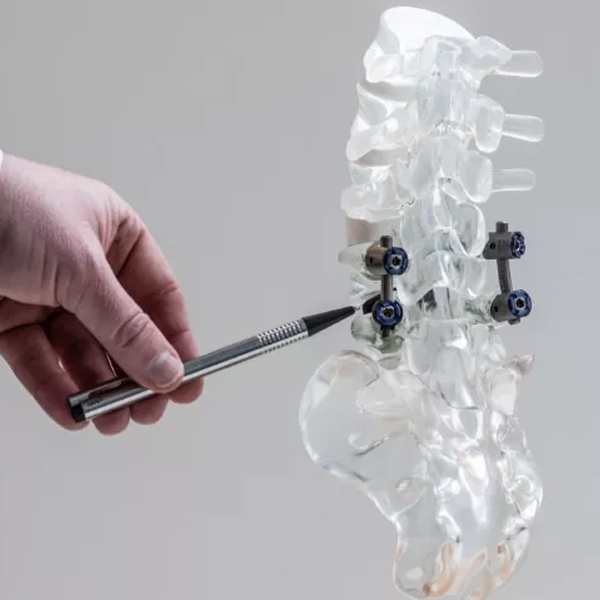
Screws (pedicle screws) are inserted into the vertebrae on either side at each level (with X-ray guidance to ensure correct placement). These screws are then connected with rods to hold the vertebrae in alignment.
If doing an interbody fusion (often done nowadays as it adds stability), part of the disc is removed and a cage (spacer filled with bone graft) is inserted into the disc space between vertebrae to restore height and help fusion.
Bone graft – which could be the patient’s own bone from decompression, and/or cadaver donor bone, or synthetic materials – is placed around the area: in the disc space and/or along the back of the spine.
Once everything is in place, the hardware is tightened to hold the spine. X-rays confirm alignment. Then layers are closed; possibly a drain is placed to collect any excess blood.
For an anterior approach (like ACDF in the neck or ALIF in the lumbar spine), the surgeon goes through the front, removes the disc, inserts a graft/cage, and often adds a plate and screws in front or does supplemental screws from the back.
The specifics vary, but the concept is: rigid fixation + bone graft = eventual fusion.

OneTreeHealth
Fusion is a bigger surgery, so hospital stay might be 2–3 days (for 1–2 level lumbar, maybe home in 2 days; for more levels or older patients, sometimes longer). Pain will be more than a simple laminectomy because of more muscle dissection and hardware. You’ll have IV pain meds initially, transitioning to orals.
Possibly a brace (some surgeons use a lumbar brace or neck collar to remind patients to limit motion while fusing; others feel hardware is enough). You’ll be encouraged to get up and walk the next day (with physical therapy help). Walking is good for recovery and circulation (and fusion healing).
Initially, avoid bending, lifting anything more than a few pounds, or twisting – basically keep the spine relatively straight and stable while healing. If you have a drain, it’s usually removed day 1–2. You may have a urinary catheter from surgery that comes out the next day.
Once you can move safely, pain is controlled with pills, and you’re eating, you can go home.
At home: You’ll need rest and help with some tasks for a couple of weeks. Walking frequently is encouraged, but no strenuous activity. Incision care as directed (keep it dry until follow-up). You’ll follow up ~2 weeks for wound check, and possibly X-rays at intervals (6 weeks, 3 months, etc.) to monitor fusion progress.
Fusion itself takes months to solidify (around 3–6 months for significant healing, and up to 12–18 months for complete fusion mass to form). In that time, you must avoid smoking (absolutely) and follow guidelines on activity.
Typically, at 6 weeks, you might start gentle physical therapy focusing on mobility and core without stressing the fusion. By 3 months, bone is starting to fuse; you may increase activities but still avoid heavy lifting or high impact until cleared (~6+ months).
Long term: The fused segment won’t move, but the levels above and below will take more load, so your surgeon might advise maintaining a strong core and avoiding extreme sports to protect adjacent levels.
With a successful fusion, patients often have significantly reduced pain (particularly if it was instability pain or nerve pain from a slip), but might notice a slight decrease in flexibility in that area (e.g., if you fuse L4–L5, some bending motion is lost, but many don’t notice dramatically).
Benefits
Benefits include:
<img src="https://www.onetreehealth.com/wp-content/uploads/2025/08/CITYPNG.COMHD-Circle-Green-Tick-Mark-Symbol-Icon-PNG-1500x1500-1-300x300.png" alt="" width="31" height="31" Stability: A painful or unstable spinal segment is stabilized, which can relieve pain that was caused by micro-motions or vertebrae slipping. For instance, patients with spondylolisthesis often feel much better because the vertebra is no longer sliding and irritating nerves.
<img src="https://www.onetreehealth.com/wp-content/uploads/2025/08/CITYPNG.COMHD-Circle-Green-Tick-Mark-Symbol-Icon-PNG-1500x1500-1-300x300.png" alt="" width="31" height="31" Pain Relief: Especially if the fusion was done for degenerative disc pain or severe arthritis, eliminating motion can take away that pain generator. Similarly, nerve pain that was due to compression plus instability often improves because the nerve is decompressed and the environment is stable.
<img src="https://www.onetreehealth.com/wp-content/uploads/2025/08/CITYPNG.COMHD-Circle-Green-Tick-Mark-Symbol-Icon-PNG-1500x1500-1-300x300.png" alt="" width="31" height="31" Correcting Deformity: Fusions can straighten and hold the spine if done for scoliosis or kyphosis, improving posture and possibly lung function, appearance, etc.
<img src="https://www.onetreehealth.com/wp-content/uploads/2025/08/CITYPNG.COMHD-Circle-Green-Tick-Mark-Symbol-Icon-PNG-1500x1500-1-300x300.png" alt="" width="31" height="31" Preventing Further Nerve Damage: By stabilizing, you might protect nerves from ongoing compression or stretch.
<img src="https://www.onetreehealth.com/wp-content/uploads/2025/08/CITYPNG.COMHD-Circle-Green-Tick-Mark-Symbol-Icon-PNG-1500x1500-1-300x300.png" alt="" width="31" height="31" Long-Term Solution: Once fused, that segment generally doesn’t cause trouble again (no disc to herniate, no joint to move). It’s a permanent fix for that level’s issues.
<img src="https://www.onetreehealth.com/wp-content/uploads/2025/08/CITYPNG.COMHD-Circle-Green-Tick-Mark-Symbol-Icon-PNG-1500x1500-1-300x300.png" alt="" width="31" height="31" Function Improvement: Many can return to normal activities (sans extreme spine twisting perhaps) without the pre-op pain. People who had neurological deficits may see improvement if nerves heal after being stabilized and decompressed.
Risks
<img src="https://www.onetreehealth.com/wp-content/uploads/2025/08/CITYPNG.COMHD-Circle-Green-Tick-Mark-Symbol-Icon-PNG-1500x1500-1-300x300.png" alt="" width="31" height="31" Non-union (Failed Fusion): The bones may not fuse solidly – this is called a pseudarthrosis. It can happen in some cases (higher risk if multi-level, if you smoke, have diabetes, or poor bone quality). If it doesn’t fuse and you’re still in pain, sometimes a revision surgery is needed to try again with more bone graft or different techniques. Hardware often can maintain stability if one level doesn’t fully fuse, but it may cause pain or hardware breakage over time if not fused.
<img src="https://www.onetreehealth.com/wp-content/uploads/2025/08/CITYPNG.COMHD-Circle-Green-Tick-Mark-Symbol-Icon-PNG-1500x1500-1-300x300.png" alt="" width="31" height="31" Adjacent Segment Disease: Fusing one segment puts more stress on the next ones. Over years, those levels might degenerate faster, potentially leading to new issues maybe 5–10+ years down the line. For example, after an L4–L5 fusion, later one might get a herniation at L3–L4. It’s a known long-term risk.
<img src="https://www.onetreehealth.com/wp-content/uploads/2025/08/CITYPNG.COMHD-Circle-Green-Tick-Mark-Symbol-Icon-PNG-1500x1500-1-300x300.png" alt="" width="31" height="31" Hardware Complications: Screws or rods can break or loosen, especially if fusion isn’t achieved. Sometimes hardware causes irritation (very rarely, you feel a screw or it impinges something). Usually hardware stays for life, but if it causes issues—or if fusion is achieved and hardware is bothersome—it can be removed (uncommon).
<img src="https://www.onetreehealth.com/wp-content/uploads/2025/08/CITYPNG.COMHD-Circle-Green-Tick-Mark-Symbol-Icon-PNG-1500x1500-1-300x300.png" alt="" width="31" height="31" Infection: A fusion (especially with hardware) has a risk of deep infection, which might necessitate antibiotics or even hardware removal in severe cases. It’s higher risk than a simple discectomy, but still relatively low (~2–4%). Surgeons give IV antibiotics and operate in clean conditions to minimize this.
<img src="https://www.onetreehealth.com/wp-content/uploads/2025/08/CITYPNG.COMHD-Circle-Green-Tick-Mark-Symbol-Icon-PNG-1500x1500-1-300x300.png" alt="" width="31" height="31" Bleeding: Depending on levels fused, blood loss could be moderate. Transfusions are sometimes needed in bigger fusions, but not usually for one level. They take precautions (cell saver, etc.). Hematoma risk is similar to laminectomy
<img src="https://www.onetreehealth.com/wp-content/uploads/2025/08/CITYPNG.COMHD-Circle-Green-Tick-Mark-Symbol-Icon-PNG-1500x1500-1-300x300.png" alt="" width="31" height="31" Nerve Injury: The risk is present just like in laminectomies, since often decompression is part of it. Also, placing screws has a small risk of hitting a nerve root. In cervical anterior fusions, there’s risk to the spinal cord or nerve roots if not careful. But typically, risk of major neuro injury is low—a few in 1,000 chance, depending on complexity
<img src="https://www.onetreehealth.com/wp-content/uploads/2025/08/CITYPNG.COMHD-Circle-Green-Tick-Mark-Symbol-Icon-PNG-1500x1500-1-300x300.png" alt="" width="31" height="31" Pain Not Fully Relieved or New Pain: Fusion addresses mechanical pain and nerve compression, but sometimes back pain can persist if there are other issues. Some patients can have ongoing pain even if fusion is solid—nerve scarring, muscle pain, or adjacent issues can contribute. Also, loss of motion at the fused segment can cause stiffness—e.g., neck fusion might limit turning a bit, which some might perceive as discomfort or limitation
<img src="https://www.onetreehealth.com/wp-content/uploads/2025/08/CITYPNG.COMHD-Circle-Green-Tick-Mark-Symbol-Icon-PNG-1500x1500-1-300x300.png" alt="" width="31" height="31" General Surgical Risks: Blood clots, anesthesia complications, etc. With bigger surgery, clot risk is there; prophylactic blood thinners or compression devices are often used.
<img src="https://www.onetreehealth.com/wp-content/uploads/2025/08/CITYPNG.COMHD-Circle-Green-Tick-Mark-Symbol-Icon-PNG-1500x1500-1-300x300.png" alt="" width="31" height="31" Throat Issues in ACDF: If cervical, temporary swallowing difficulty or hoarseness is common since the esophagus is moved and the vocal cord nerve may be manipulated. Usually resolves, but rarely could be long-term.Frequently Asked Questions:
Generally, initial bone healing starts in about 6 weeks, with significant progress by 3 months. Often by 6 months, you have a solid fusion mass forming. However, the complete fusion process can continue up to a year or more.
We will schedule follow-up X-rays at intervals (like at 3 months, 6 months, and 12 months). On X-ray—or sometimes a CT scan—we look for bridging bone between vertebrae and no motion on flexion-extension X-rays to confirm fusion. The hardware holds things steady in the meantime.
You physically won’t “feel” the fusion happen (some think they’ll wake up one day fused – it’s gradual), but over time you might feel more confident movement-wise as any initial micro-motions that cause pain stop.
The doctor will eventually declare you “fused” when imaging shows solid bone connections. Until then, you should follow precautions—particularly avoiding smoking and adhering to movement restrictions
In the vast majority of cases, the hardware stays in permanently. It’s made of titanium or similar material, which is compatible with your body. Once the bone fuses, the hardware is kind of redundant, but we don’t remove it unless there’s a problem—because that would be another surgery.
Most people do not feel their hardware. In the lumbar spine, it’s deep enough and muscles cover it. Very thin patients might feel a bit of rod prominence under the skin in some cases, but it’s not common.
In the neck, a plate is in front of the spine, behind the esophagus—you won’t feel that (except maybe some slight thickness when swallowing until you get used to it, but usually not). People often forget they have screws/rods.
It should not set off metal detectors typically (small amount of metal, plus TSA is used to spine hardware). If by chance hardware causes discomfort or if screws impinge on a nerve (rare but can happen if screw position was off), then revision or removal might be considered, but that’s uncommon.
We give you a medical card about your implant if you need it for travel or MRI info.
It depends on the level and how many. One-level lumbar fusion (like L4–L5) results in a very minimal loss of overall lumbar motion – your spine has multiple levels of motion, so losing one still leaves flexibility. Many patients don’t notice any difference in daily life activities.
Multi-level fusions add up; e.g., fusing L4–S1 (two levels) you might notice it a bit when bending (but hips also provide much bending motion, so you adapt).
In the cervical spine, fusing one or two levels out of seven doesn’t typically cause big range of motion issues – you might have slightly reduced turning or bending, but other levels compensate some. For instance, after a single-level ACDF, most return to normal tasks; perhaps if you fuse multiple levels (C3–7), you’ll definitely have a stiffer neck and may need to turn more from the torso.
Your surgeon can give specifics; usually they say for one level, minimal impact, for multi-level, moderate impact. Regardless, most people consider the trade-off worth it to relieve pain or improve stability.
Physical therapy can also help maximize flexibility in the unfused segments and improve overall posture.
If preserving motion is a huge concern (like in the neck for a younger patient), sometimes artificial disc replacement is an alternative at some levels—but that’s another topic.
For lumbar spine, especially low down (L5–S1), that segment doesn’t contribute a ton to flexion (most comes from hips and upper lumbar), so fusing it often isn’t much perceived.
Yes, once you’re healed. In fact, we encourage returning to a healthy, active lifestyle—with some modifications.
Low-impact activities are generally fine (walking, swimming, cycling, elliptical). Many patients get back to golfing, hiking, etc., after a lumbar fusion once healed (~6+ months). High-impact or contact sports (like heavy weightlifting or football) are more questionable—they could put stress on adjacent levels. But I’ve had patients who returned to skiing moderately or playing tennis.
It depends on how extensive the fusion was and personal factors. For cervical fusions, many resume normal activities but may avoid things like high impact that risk neck injury (like tackle football).
The key is: after fusion, maintain core and overall strength to support your spine. Be mindful of any new pains—if something causes pain, modify or reduce it.
But you won’t be an invalid by any means; after recovery, you should be able to travel, exercise, and work (maybe avoid heavy manual labor if it was a multi-level fusion, but many go back to work—including physical jobs—with proper ergonomics).
Always discuss with the surgeon regarding the timeline to resume specific activities—typically, heavy lifting is restricted for maybe 3 months or more; light exercise can start earlier with guidance.
Success depends on the condition being treated. For something like degenerative spondylolisthesis with nerve compression, fusion plus decompression has a high success rate in reducing leg pain and improving function (75–90% range in studies).
For pure discogenic back pain, success rates can be lower (maybe 60–70% significantly improved), because back pain can be multifactorial. In general, if the indication was clear (instability, deformity, nerve compression), fusion outcomes are good for those issues.
It may not remove 100% of pain—often these surgeries are considered successful if pain is reduced by, say, 50% or more and function improves. Some patients get nearly complete relief; others still have some residual pain requiring occasional meds or therapy.
We set realistic expectations: the goal is substantial improvement in pain and stability. If you have nerve symptoms pre-op, those might take time to recover, and sometimes numbness or slight weakness might remain if the nerve was damaged. But preventing worsening is still a win.
We also caution that you may trade some back flexibility for less pain. Most are happy with that trade-off when pain was debilitating.
We’ll monitor your progress; success is also measured by you being able to do more and enjoy life better post-op. Keep in mind, adjacent segments could cause issues in the future—but if that happens, that’s years down the line and might require treatment then.
Right now, focus on addressing the current problem. All in all, most patients who get a fusion for the right reason are glad they did it because the debilitating pain or instability is improved and they can get back to activities, albeit with some adjustments.

Contact Us Today!
When your spine’s stability is compromised or pain from a worn-out disc just won’t relent.
One Tree Health’s neurosurgery team is here with advanced spinal fusion solutions. We know deciding on a fusion is a big step – that’s why our experts thoroughly evaluate your condition and use the latest techniques to maximize success and minimize impact on your mobility
Our goal is simple: to secure your spine and free you from the pain that’s holding you back. From state-of-the-art imaging to precise surgical execution and attentive post-op care, you’ll be in good hands every step of the way. Many of our patients return to active lives – working, playing with grandkids, enjoying hobbies – once their back or neck is stabilized and healed.
You don’t have to endure constant pain or fear of your spine “slipping” any longer. Schedule a consultation with One Tree Health to discuss whether a spinal fusion is the right step for you. We’ll answer all your questions and tailor a plan to your unique needs, ensuring you feel confident and supported on the road to recovery. Take control of your spine health and get back to living life on your terms.
Contact us today – let’s work together to build a stronger, pain-free foundation for your future.
OneTreeHealth provides coordinated, compassionate care for patients recovering from injury specializing in orthopaedics, neurology, surgery, interventional pain management, and more. We simplify the recovery journey by managing care under one roof, so patients can focus on healing.
Useful Links
Reach Us
397 Wallace Rd Nashville, TN 37211 Suite#303
(615) 696-9900
hello@onetreehealth.com
Copyright 2025, One Tree Healthcare. All Rights Reserved.

