Orthopedic Surgery
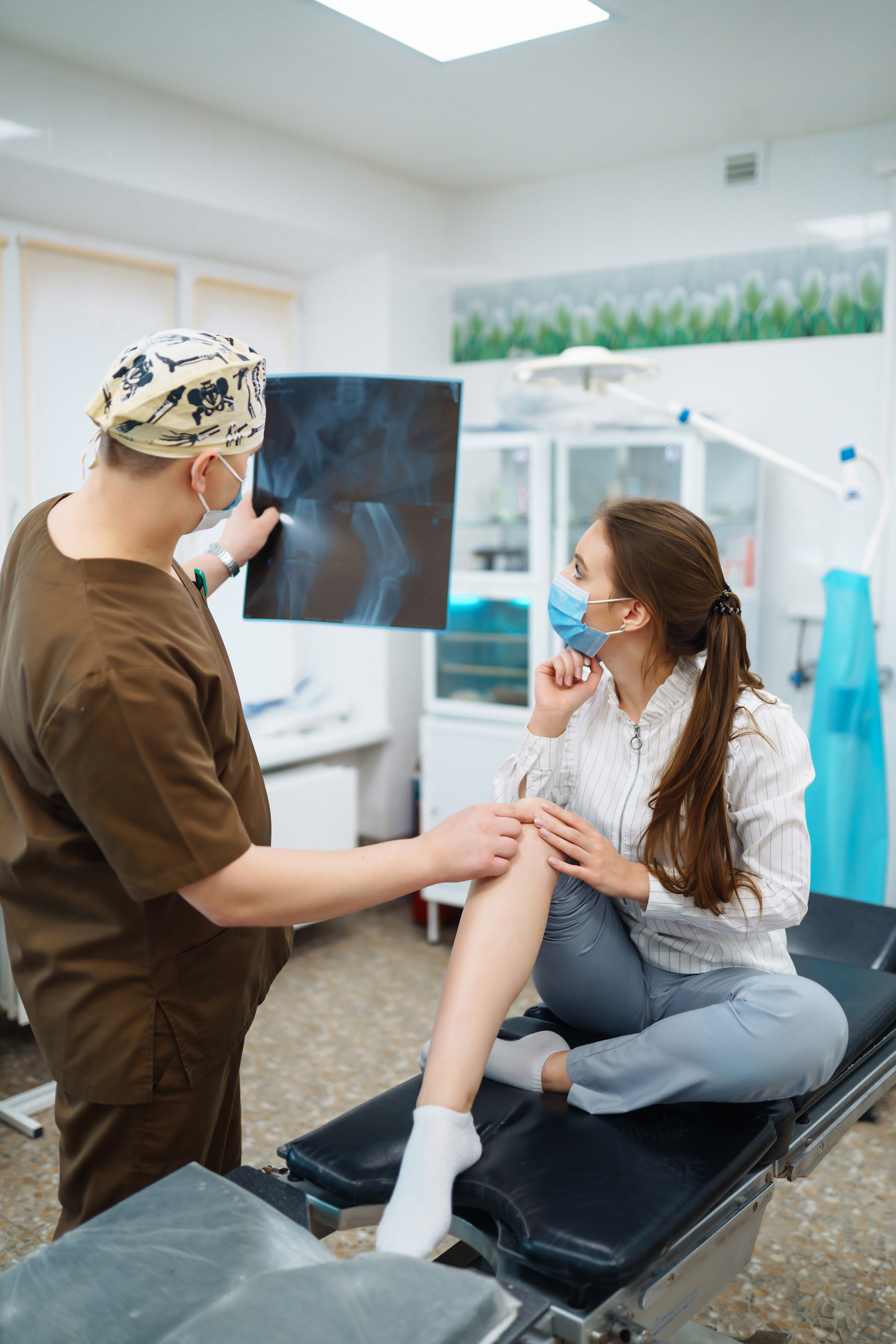
Introduction: Orthopedic Surgery
Life is motion – and Orthopedic Surgery at One Tree Health is all about keeping you moving, pain-free, and doing the activities you love. Our orthopedic team treats injuries and disorders of the bones, joints, muscles, and ligaments. We understand that an orthopedic problem (like a bad knee or an injured shoulder) doesn’t just hurt — it can stop you from working, exercising, or even playing with your kids. That’s why we take a personalized, patient-centered approach to orthopedic care. Whether you’re a weekend warrior with a sports injury or someone dealing with arthritis in your hip, we’re here to offer the latest treatments with a caring touch.
Our orthopedic surgeon(s) are skilled in both minimally invasive techniques and complex surgical reconstructions, so we can tailor the solution to the severity of your condition. We always consider conservative treatments first — such as physical therapy, medications, or injections — and many of our patients improve without surgery. But if you do need an operation, rest assured you’re in capable hands. We prioritize techniques that minimize incision size, reduce pain, and speed up recovery (like arthroscopy for many joint repairs). We’ll walk you through the entire process: what the surgery entails, how to prepare, and what recovery will look like. At One Tree Health, orthopedic care is a team effort — our surgeons, pain specialists, and physical therapists coordinate closely to ensure you get comprehensive care from injury through rehabilitation.
Conditions We Treat
Our Orthopedic Surgery department handles a wide array of musculoskeletal issues, including:
Sports Injury
Sprains, strains, and tears we treat them all. From ACL tears in the knee to rotator cuff tears in the shoulder, meniscus injuries, Achilles tendon ruptures, and more.
If you’ve injured yourself on the field, court, or in the gym, we can help evaluate and manage it. Some injuries may heal with rest and therapy; others might need surgical repair.
We’re experienced in sports medicine principles and will tailor care to get you safely back to your sport.
Joint Pain & Arthritis
Chronic knee pain from osteoarthritis, a hip that’s stiff and painful, or shoulder arthritis — these wear-and-tear conditions are common, and we offer both non-surgical and surgical solutions.
When conservative measures (like medication, injections, or therapy) aren’t enough, we can discuss surgical options such as joint arthroscopy or even joint replacement for more severe cases.
Our focus is on pain relief and restoring function so you can walk, climb stairs, get dressed, and live without debilitating joint pain.
Fractures (Broken Bones)
We treat fractures of the upper and lower extremities, as well as certain spine fractures in coordination with neurosurgery.
Whether it’s a simple broken wrist or a complex leg fracture, we provide prompt, expert care. Some fractures can be treated with casting or bracing, while others may require surgery (open reduction and internal fixation — ORIF).
In surgical fracture repair, we use plates, screws, rods, or pins to realign and stabilize the bone so it heals correctly. Our orthopedic surgeon ensures your bones are set properly for optimal recovery.
We also manage fracture complications or non-unions — bones that haven’t healed as expected.
Shoulder Conditions
From rotator cuff tears and shoulder impingement to dislocations and labrum tears (like SLAP tears), we’ve got you covered.
We often utilize arthroscopic shoulder surgery, which involves a tiny camera and instruments inserted through small incisions to repair tissues such as tendons, ligaments, and cartilage. This minimally invasive approach typically results in less pain and faster rehabilitation than traditional open surgery.
For severe shoulder arthritis, we also offer shoulder replacement surgery — including both anatomic and reverse total shoulder arthroplasty.
Knee Conditions:
We treat ACL injuries, meniscus tears, cartilage defects, kneecap (patella) problems, and arthritis.
Many knee issues can be addressed with knee arthroscopy — a minimally invasive procedure using a small camera to trim a torn meniscus or smooth damaged cartilage.
For athletes with a torn ACL, we perform ACL reconstruction, replacing the torn ligament with a graft to restore knee stability.
For patients with advanced arthritis, we may recommend knee replacement surgery. If it’s not performed directly at our center, we’ll coordinate care to ensure a seamless referral and recovery process.
s.
Hip Conditions
Hip labral tears, impingement (FAI), and mild arthritis can sometimes be treated with arthroscopic hip surgery, a minimally invasive approach to repair damage and relieve pain.
Hip fractures, which are common in older adults after falls, are considered surgical emergencies. We manage these at our affiliated hospitals using either internal fixation or partial hip replacement, depending on the type of fracture.
For patients with significant hip arthritis, total hip replacement is a highly effective treatment. We ensure that anyone who needs it receives the proper surgical care and support throughout recovery.
Hand, Wrist, and Elbow
We treat common upper extremity issues such as carpal tunnel syndrome (often with a simple outpatient carpal tunnel release), trigger fingers, wrist fractures, and tennis elbow (when surgery is needed).
Many of these conditions can be managed on an outpatient basis with quick recovery times, helping you return to your daily activities with minimal disruption.
Foot & Ankle Care
We treat a range of foot and ankle conditions including ankle sprains and fractures, Achilles tendon injuries, plantar fasciitis, and bunions.
While some foot and ankle issues may be referred to a podiatric specialist, our orthopedic surgeon can manage many traumatic and chronic conditions — from fixing an ankle fracture with plates and screws to repairing an Achilles tendon rupture.
In essence, if it involves the musculoskeletal system, our Orthopedic team can evaluate it and either treat it or direct you to the appropriate care. We emphasize a holistic approach – treating the injury and also guiding your rehabilitation to prevent future
issues.
Orthopedic Procedures and Treatments
Here are some key procedures and treatments you’ll find in our orthopedic department:
OneTreeHealth
Arthroscopy (Minimally Invasive Surgery)
Arthroscopy is a minimally invasive procedure where a small camera (arthroscope) is inserted into a joint through tiny incisions to diagnose and treat joint problems. We commonly use it for the knee (meniscus tears, ACL reconstruction), shoulder (rotator cuff and labrum repairs, impingement), and occasionally the ankle, wrist, or hip.
Benefits include smaller incisions, less pain, and faster recovery compared to open surgery. Most procedures are outpatient — meaning you go home the same day. For example, arthroscopic rotator cuff repair uses just a few small incisions to reattach the tendon to bone. Recovery is easier, and physical therapy typically starts shortly after.

OneTreeHealth
ACL Reconstruction
The ACL (anterior cruciate ligament) is a key stabilizer of the knee and is often torn during sports. Our orthopedic surgeon performs minimally invasive ACL reconstruction, typically using arthroscopy. A graft — from your hamstring, patellar tendon, or a donor — is used to create a new ligament and secured with screws or fixation devices.
It’s an outpatient procedure, so you go home the same day with a leg brace. Rehab begins right away with gentle exercises and progresses over several months. While full return to sports takes about 6–9 months, most patients are back to normal daily activities much sooner. ACL surgery is highly effective in restoring knee strength and stability.

OneTreeHealth
Rotator Cuff Repair
The rotator cuff is a group of shoulder tendons that help you lift and rotate your arm. Tears are common due to aging or injury and often cause pain and weakness.
We usually start with physical therapy, but if the tear is large or not improving, arthroscopic rotator cuff repair may be recommended. This outpatient procedure uses small incisions to re-anchor the torn tendon to the bone with suture anchors (tiny screws with stitches).
After surgery, the arm is typically kept in a sling for 4–6 weeks, followed by physical therapy to restore motion and strength. Most patients experience significant pain relief and better shoulder function, with full recovery taking a few months of rehab.
OneTreeHealth
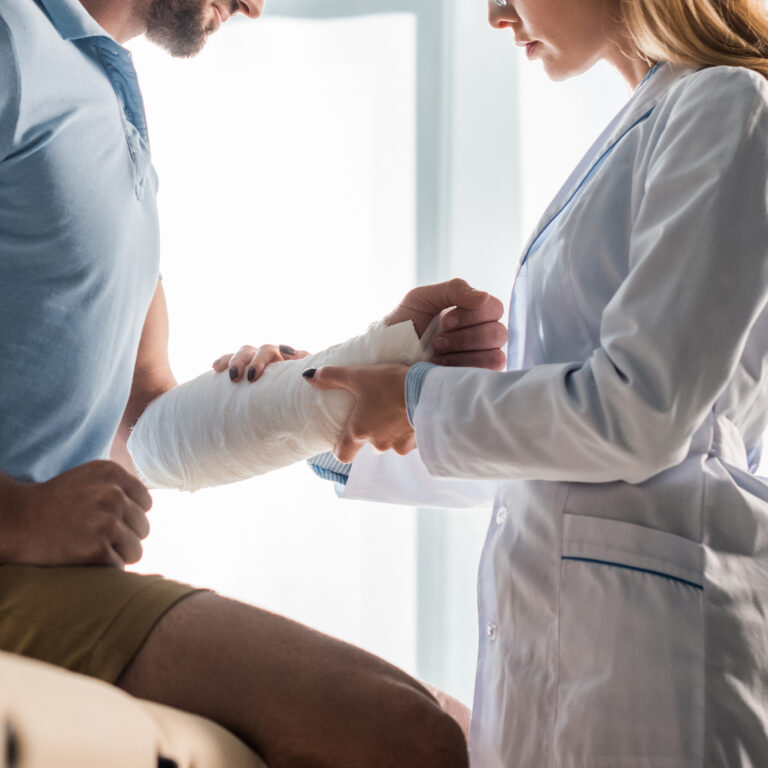
Fracture Repair (Open Reduction and Internal Fixation - ORIF)
For fractures that are displaced or unlikely to heal properly with a cast, we perform ORIF — a surgical procedure where we realign the broken bone (open reduction) and secure it using internal hardware like plates, screws, or rods (internal fixation).
For example, a badly broken ankle may require an incision to reposition the bones and stabilize them with a plate and screws. ORIF is commonly used for hip, wrist, ankle, and certain shoulder fractures. Most bones heal in 6–8 weeks, and the hardware typically stays in permanently unless it causes discomfort. Our goal is to create a stable repair, allow for early movement, and minimize complications. Healing is monitored through follow-up X-rays.
OneTreeHealth
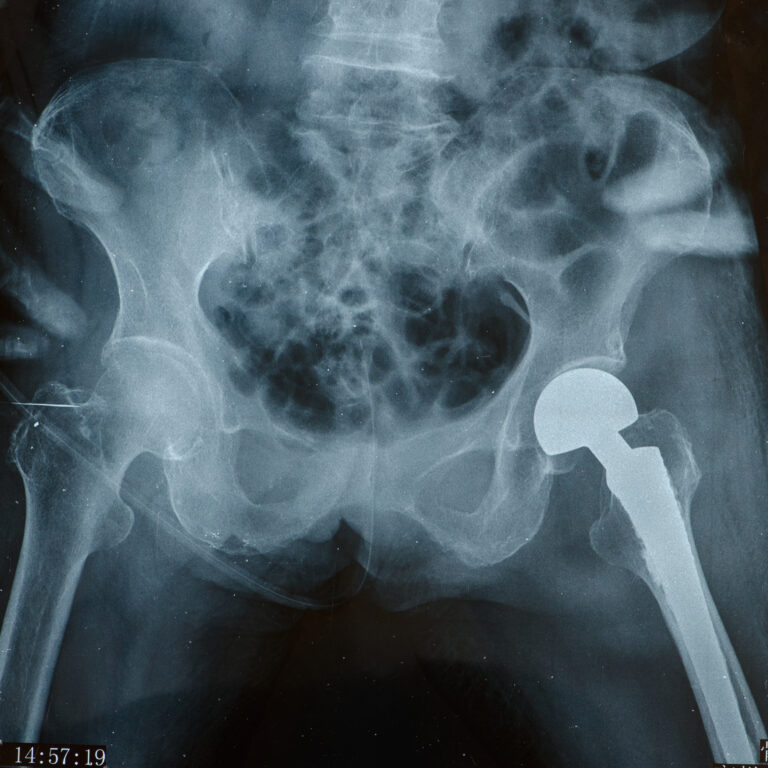
Joint Replacement (Arthroplasty):
While we prioritize joint-preserving treatments, sometimes joint replacement is the best option for severe arthritis.
We perform shoulder replacements in-house and coordinate with trusted partners for knee and hip replacements when needed. In these procedures, the damaged ends of the bones are removed and replaced with artificial components (metal, ceramic, or plastic) to restore smooth joint function.
For example, in a total knee replacement, the ends of the femur and tibia are resurfaced with metal and a plastic spacer is placed in between. These surgeries offer excellent pain relief and improved mobility, though recovery involves a short hospital stay and several weeks of physical therapy.
If you’re a candidate, we’ll guide you through the entire process with thorough education and personalized support.
OneTreeHealth
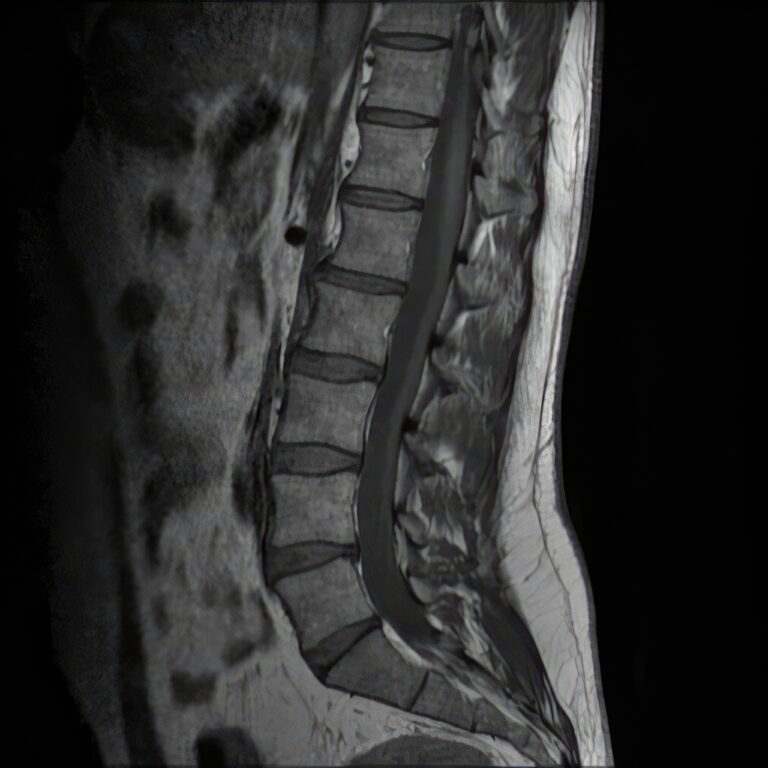
Spine Surgery (Orthopedic Approach)
Our orthopedic spine surgeon treats many spinal conditions similarly to a neurosurgeon, offering procedures such as discectomies, laminectomies, spinal fusions, and artificial disc replacements.
The best approach depends on your specific condition. For example, an artificial disc replacement in the neck may be recommended instead of a fusion to preserve mobility in the right candidate.
Whenever possible, we use minimally invasive techniques — including smaller incisions and muscle-sparing approaches — to reduce pain and speed up recovery.
We also work closely with pain management to support your care before and after surgery, including options like injections, bracing, and physical therapy. Spine surgery recovery varies by procedure, but our team ensures you have a clear plan and support every step of the way.
OneTreeHealth
Platelet-Rich Plasma (PRP) and Other Injections
In addition to surgeries, our ortho team can provide injections for certain conditions. PRP injections (using your own blood growth factors) can be considered for chronic tennis elbow, knee arthritis, or other tendon issues if appropriate, as emerging evidence suggests some benefit.
We also do corticosteroid injections into joints (like shoulders, knees) for pain relief, often in conjunction with therapy – this can delay or even negate the need for surgery in some cases.
OneTreeHealth
Casting, Splinting, and Durable Medical Equipment
Not everything needs an operation. We do plenty of fracture care with casting or splints when appropriate
(like many wrist fractures, small finger/toe fractures, etc.), and provide bracing for sprains or chronic conditions (like knee braces for arthritis, ankle braces for instability).
Our clinic can fit you with the right gear (slings, walking boots, crutches, etc.) and teach you how to use it.
Frequently Asked Questions:
Orthopedic Surgery
Many orthopedic issues can heal or improve without surgery. We always
assess if conservative treatments could work first. For example, a meniscus tear
in the knee might be managed with rest, meds, and therapy if it’s small and your
symptoms aren’t too bad. Fractures often heal in casts without surgery if they’re
well-aligned and stable. We recommend surgery when we believe it’s truly the
best way to fix the problem or when non-surgical methods have failed. If you’re
unsure, feel free to ask about a trial of non-operative care. We can often set a
timeframe – like “let’s try 6 weeks of therapy, and if the shoulder is still frequently
dislocating, then consider surgery.” We want you to be comfortable with the plan,
and we don’t operate unless it’s necessary for your recovery or relief.
All surgeries carry some risks, and orthopedics is no different. General risks
include infection (we give antibiotics around surgery to prevent this), bleeding
(usually minimal in ortho, but we cauterize vessels during surgery), blood clots
(particularly for leg surgeries – we often use blood thinners or encourage early
mobilization to reduce this risk), and anesthesia risks. Then there are specific
risks: for joint repairs, sometimes the repair might not heal fully or could re-tear
(rotator cuff re-tear in a small percentage of cases, for instance). For fracture
surgeries, there’s a risk the bone might take longer to heal or not heal (non-
union) which might need further treatment. Nerve or blood vessel injury is very
rare but a known risk depending on location (we’re extremely careful with
surgical technique to avoid this). We’ll go over the particular risks of your surgery
with you beforehand, so you’re aware. Keep in mind, by using modern
techniques and having skilled surgeons, the complication rates are quite low. And
doing nothing also has “risks” – e.g., a torn ACL not fixed can lead to knee
instability and further damage. We weigh those considerations carefully.
We focus heavily on pain management to keep you comfortable. Orthopedic
surgeries can cause some post-op pain, particularly in the first few days, but we
use multimodal pain control. That means we often use a combination of: nerve
blocks (which can numb the area for hours or even a day), anti-inflammatory
meds, acetaminophen, icing, and carefully prescribed opioids for breakthrough
pain. We might also recommend elevation and rest to reduce swelling, which
helps pain. Patients often find the pain is manageable and improves significantly
within a few days. For something like joint replacement or larger surgeries, the
pain might be more, but physical therapy and medications work together to
control it. We’ll ensure you have adequate pain relief before sending you home.
And we’ll follow up to adjust any medications if you’re struggling. Remember,
pain is expected to some degree – but our goal is to keep it at a tolerable level so
you can sleep, move, and participate in therapy.
It depends on the surgery and which side (for legs, driving is affected). A
general rule is: you can drive when you are no longer on narcotic pain meds
and when you can operate the vehicle safely (which includes having enough
mobility and strength in the limb). For example, after a right knee surgery, you
usually shouldn’t drive for at least a few weeks because you need to be able to
brake quickly. After left knee surgery (and you have an automatic car), you might
drive sooner, maybe 1-2 weeks, if off pain meds. For upper extremity, say right
shoulder surgery, you have to be careful because you may not have full control
with one arm – typically waiting at least until you’re out of a sling and can use
that arm in front of you. We will give you personalized guidance. Safety is key;
you must be confident you can react normally to drive. And never drive under the
influence of pain medications stronger than Tylenol or ibuprofen. We’ll clear you
when it’s appropriate during follow-ups.
In many cases, yes, physical therapy (PT) is an integral part of recovery. The
frequency and duration vary. For something like an ACL reconstruction, PT is
often 2-3 times per week for 3-4 months (with home exercises on other days) and
then gradually tapering to independent exercise. For a simple arthroscopy (like
trimming a meniscus), you might only do a few sessions to learn exercises and
then continue on your own. For rotator cuff repair, therapy usually starts a couple
weeks after surgery and goes for 2-3 months to regain full motion and strength.
Fractures that were casted often need some PT after the cast comes off to
restore mobility. We’ll prescribe what’s appropriate, and the therapists will
regularly send us progress notes. You are a big part of therapy success – doing
your home exercises and following guidelines significantly influences your
outcome. We can’t stress enough that PT is often as important as the surgery
itself for a good result! But don’t worry, we’ll be with you, adjusting your therapy
plan if needed and making sure you’re progressing. If formal PT is not needed
(some minor procedures don’t require it), we’ll give you instructions for home
care.
Have more questions? Check out our Full FAQ page for answers about appointments,
treatments, recovery, and more.



Contact Us Today!
If you’re ready to move better and hurt less, reach out to us.
The bottom line: our Orthopedic team is dedicated to helping you heal fully and get back to an active life. We’ll evaluate your condition and craft a plan that fits your goals, whether it’s conservative care or surgical repair.
Schedule an Appointment with our orthopedic specialist today and take the first step toward getting back in action. At One Tree Health, we’re committed to keeping you strong, mobile, and doing what you love.
OneTreeHealth provides coordinated, compassionate care for patients recovering from injury specializing in orthopaedics, neurology, surgery, interventional pain management, and more. We simplify the recovery journey by managing care under one roof, so patients can focus on healing.
Useful Links
Reach Us
397 Wallace Rd Nashville, TN 37211 Suite#303
(615) 696-9900
hello@onetreehealth.com
Copyright 2025, One Tree Healthcare. All Rights Reserved.

